Every nurse runs a head to toe assessment on every patient, every shift. Miss a step, and you can miss a stroke, a clot, or a pressure injury forming under the sheets.
This guide is the single reference you can scroll through at the bedside. You get the definition, prep, techniques, the full checklist by body system, documentation rules, and how AI now takes the charting off your plate.
What a Head-to-Toe Assessment Is in Nursing Practice
A head to toe assessment is a systematic, top-down physical exam that checks every major body system in the same order, every time. Nurses use it to set a baseline at admission, to catch changes at the start of a shift, and to confirm a patient is stable after a procedure.
A typical shift assessment on a stable patient takes 10 to 15 minutes. A full admission assessment can run 25 to 30 minutes because it includes a complete history and medication review.
Not every assessment has the same purpose. There are three common types, and knowing which one you are doing shapes how deep you go.
Complete Health Assessment
This is the full baseline. You do it on admission, at annual physicals, or any time a patient enters a new care setting. Every system gets examined in sequence, and you spend real time on history.
Problem-Focused Assessment
This one is narrow. The chief complaint drives where you look. Chest pain sends you straight to the cardiopulmonary exam. New weakness sends you to a neuro focus. You still scan the rest, but you zoom in on the system in question.
Ongoing Shift Assessment
Most bedside RNs mean this one when they say “head to toe.” It is the abbreviated version you run at the start of every 12-hour shift. The goal is to set your own baseline so any change later in the shift stands out.
Equipment and Patient Preparation Before Starting
Good preparation is where new nurses lose the most time. You assemble tools, set up the room, and get the patient on board before you ever place a stethoscope.
Required Equipment Checklist
Keep this kit ready at the bedside:
Stethoscope
Penlight
Thermometer
Blood pressure cuff
Pulse oximeter
Watch with a second hand
Gloves and hand sanitizer
Reflex hammer
Tuning fork
Tongue depressor
Tape measure
Snellen chart

Most hospitals stock these on the medication cart or at the bedside. If your unit is missing anything, grab it before you walk in. Stepping out mid-exam breaks patient trust and wastes time.
Setting Up the Environment
Close the curtain. Get the room warm, since your patient will be partially exposed. Raise the bed to your waist height to protect your back. Good lighting is not optional for skin and eye checks.
Patient Identification and Consent
Verify two identifiers: name and date of birth. Then explain what you are about to do in plain language, and ask for verbal consent. For sensitive exams, offer a chaperone.
Infection Control Steps
Wash your hands before and after contact, every time. Wear PPE that matches the patient’s isolation status. Wipe your stethoscope diaphragm between patients, since it lives on your neck all day and picks up everything.
Four Core Techniques for Physical Examination
Nurses use four techniques on every exam: inspection, palpation, percussion, and auscultation (IPPA). You apply them in that order on every body system, with one famous exception you will meet below.
Inspection
Look first, always. You check color, symmetry, lesions, swelling, and signs of distress. A trained eye catches most problems before a hand ever touches the patient.
Palpation
Touch with purpose. Use your fingertips for fine detail, your palms for broad areas like the abdomen, and the back of your hand for temperature. Light palpation goes about 1 cm deep. Deep palpation goes about 4 cm, and only after light is clear.
Percussion
Tap to read what is underneath. Dull sounds sit over solid organs. Resonant sounds come from air-filled lungs. Tympanic sounds come from air in the bowel. Routine shift assessments skip percussion often, but it is a core skill for focused exams.
Auscultation
Listen with the right side of the stethoscope. The diaphragm catches high-pitched sounds like lung and bowel sounds. The bell catches low-pitched sounds like heart murmurs and bruits. Warm the metal before it touches skin. Your patient will thank you.
The one exception: on the abdomen, the order flips to inspect, auscultate, percuss, palpate. Pressing on the belly first alters bowel sounds, so you listen before you touch. This comes up on the NCLEX. Do not forget it.
Head-to-Toe Assessment Checklist by Body System
This is the core of the exam. You move top down, left to right, comparing one side to the other as you go. Run the same sequence on every patient and your brain starts catching changes you would otherwise miss.
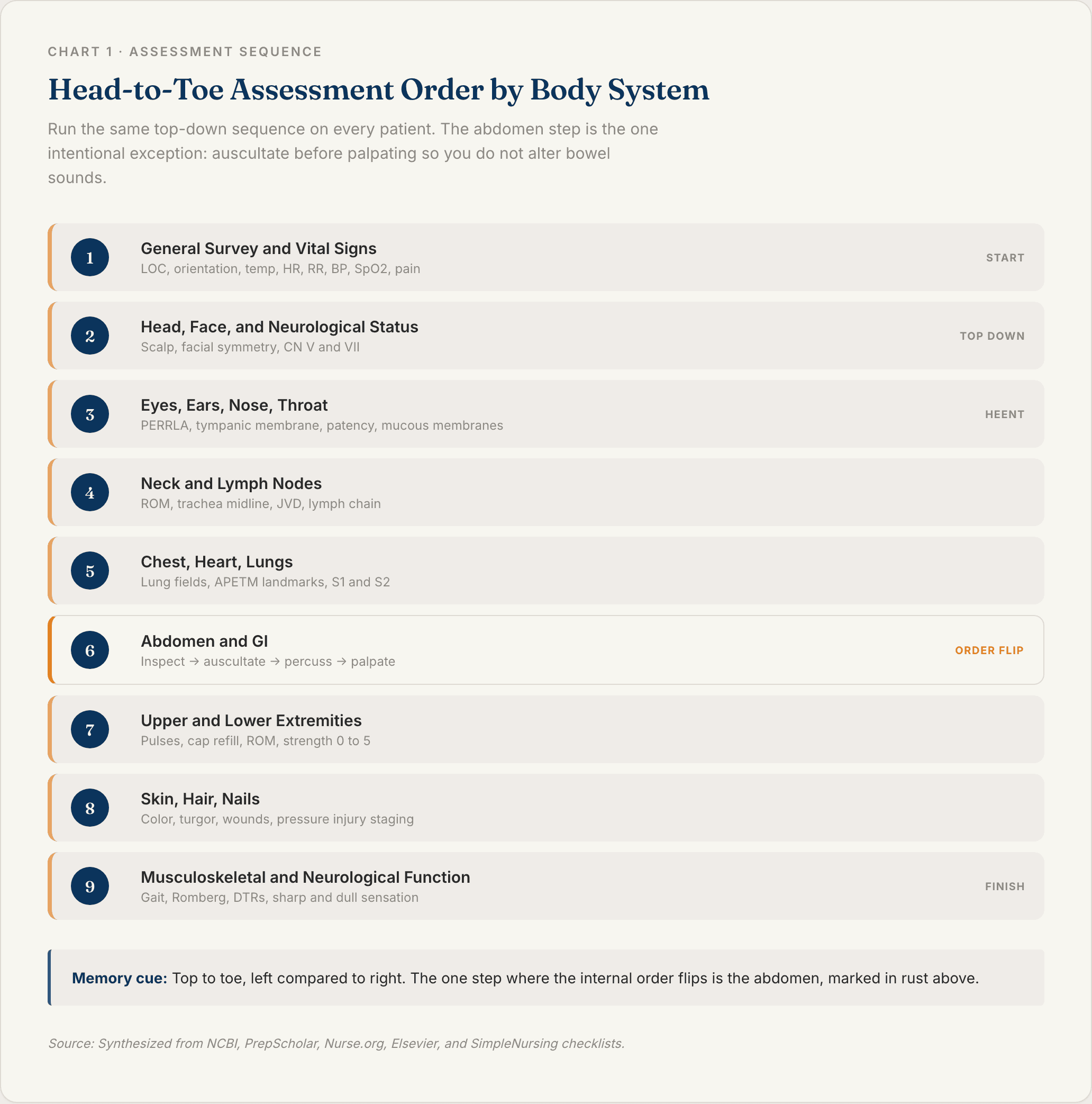
General Survey and Vital Signs
Start here before you touch the patient. You are reading the room.
Level of consciousness using AVPU or Glasgow Coma Scale
Orientation x 4 to person, place, time, and situation
General appearance, posture, gait, hygiene, affect
Vitals: temperature, heart rate, respiratory rate, blood pressure, SpO2
Pain on a 0 to 10 scale
Head, Face, and Neurological Status
Move to the scalp and face. Inspect hair distribution. Palpate the skull for tenderness and lesions. Check facial symmetry (cranial nerve VII) by asking the patient to smile and raise eyebrows. Test sharp and dull sensation on the face (cranial nerve V).
Eyes, Ears, Nose, and Throat
This is the HEENT block, and it is where new nurses tend to rush. Slow down.
Eyes: PERRLA (pupils equal, round, reactive to light and accommodation), six cardinal gazes, Snellen chart if vision is a concern
Ears: inspect the auricle, check the tympanic membrane, run a whisper test for basic hearing
Nose: confirm patency of both nostrils, check the septum is midline
Mouth and throat: moist mucous membranes, tongue midline, uvula midline, tonsils graded
Neck and Lymph Nodes
Check range of motion in all directions. Palpate the trachea, which should sit midline. Assess for jugular vein distension with the head of bed at 45 degrees. Palpate lymph nodes in order: preauricular, postauricular, occipital, submandibular, cervical chain, supraclavicular, axillary. Shoulder shrug against resistance tests cranial nerve XI.
Chest, Heart, and Lungs
Inspect the chest wall for symmetry and respiratory effort. Auscultate lung fields front and back at the apices, mid-chest, and bases. Listen to the heart at the five classic landmarks using the APETM memory hook: aortic, pulmonic, Erb’s point, tricuspid, and mitral. Note S1 and S2. Flag any murmurs, rubs, or extra sounds.
Abdomen and Gastrointestinal System
Remember the order flip here: inspect, auscultate, percuss, palpate. Listen to all four quadrants for bowel sounds before you press anywhere. Then do light palpation, and only go to deep palpation if light is painless. Ask about last bowel movement, appetite, and any nausea.
Upper and Lower Extremities
Inspect for edema, cyanosis, and lesions. Palpate pulses bilaterally: radial, brachial, femoral, popliteal, dorsalis pedis, posterior tibial. Grade each pulse 0 to 4+. Capillary refill should be under three seconds. Check range of motion and muscle strength on a 0 to 5 scale on both sides.
Skin, Hair, and Nails
Assess color, turgor, temperature, and moisture across every area you expose. Note any rashes, wounds, or pressure injuries, and stage any pressure injuries you find. Check the nail beds for color, clubbing, and capillary refill. If the patient is at risk, run a Braden score.
Musculoskeletal and Neurological Function
Observe gait and balance if the patient is ambulatory. Run a Romberg test if indicated. Check deep tendon reflexes at the biceps, triceps, patellar, and Achilles sites, and grade them 0 to 4+. Test sharp versus dull sensation and light touch on the extremities.
Documentation Standards for Nursing Assessments
An assessment you do not chart is an assessment that did not happen. Documentation turns your exam into the legal record the next nurse, the provider, and the billing team all rely on.
Objective vs Subjective Findings
Objective is what you observed, measured, or heard. Subjective is what the patient told you, and you write it in their own words using quotes. Never mix the two in the same sentence.
Example: “Patient reports ‘8 out of 10’ sharp pain in right lower quadrant. Abdomen firm to deep palpation, bowel sounds hypoactive in all four quadrants.”
SOAP Note Format
Most EHRs chart in SOAP: Subjective, Objective, Assessment, Plan. Your head to toe findings live in the Objective line. Patient-reported symptoms live in Subjective. Your clinical impression goes in Assessment. Next steps go in Plan.
Charting Abnormal Findings
Describe what you see, not what you think caused it. Write “3 cm erythematous, non-blanching area on sacrum,” not “looks like a pressure ulcer.” The provider is the one who makes the diagnosis. You notify them when a finding is outside the patient’s baseline.
Common Mistakes and Tips for a Thorough Assessment
A preceptor will tell you the checklist is only half the job. The other half is the small habits that catch problems early.
Maintaining Bilateral Symmetry Checks
Compare left to right on everything: pulses, reflexes, strength, skin color, pupil response. Asymmetry is often the first sign of a neuro or vascular issue. Assess both sides in the same breath, not with a five-minute gap in between.
Communicating Throughout the Exam
Narrate each step out loud. “I’m going to listen to your lungs now. Can you take a deep breath for me?” It calms the patient, signals professionalism, and gives you a live read on their cognitive status.
Time Management in a Busy Shift
Target 10 to 15 minutes for a routine shift assessment on a stable patient. Cluster your care: medications, assessment, and morning hygiene in a single room visit. Fewer room entries means less disruption for the patient and more time for your next task.
Modernizing Head-to-Toe Assessments with AI Support
Here is the part most assessment guides skip. Nurses spend a huge portion of every shift on documentation instead of patient care. The US has an estimated $250 billion in automatable administrative work in healthcare every year, and a big chunk of it is charting that nurses do after the patient interaction is already over.
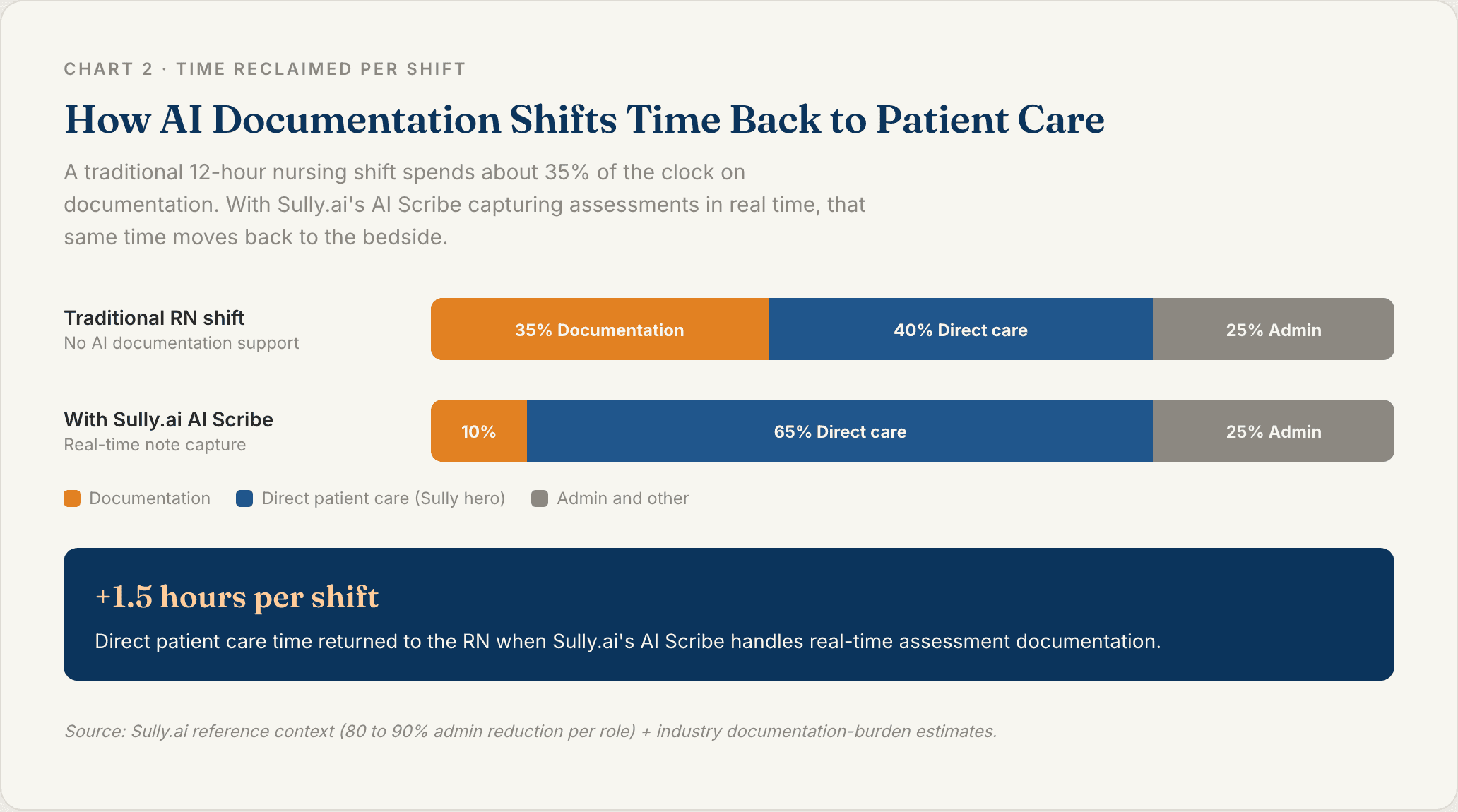
AI employees are starting to shoulder that load. They do not replace the nurse at the bedside. They take charting, intake, and scheduling off the nurse so the head to toe itself gets the full attention it deserves.
AI Scribes for Real-Time Assessment Documentation
Sully.ai’s AI Scribe captures the assessment as you narrate it. You finish the exam, the note is already in the EHR. No end-of-shift charting backlog. Sully plugs in through a single EHR integration that works with Epic, Cerner, Meditech, and Athenahealth, so you are not rebuilding the connection for every specialty.
AI Triage Nurse for Pre-Visit Intake
Sully’s AI Triage Nurse collects symptoms, history, and medication reconciliation before you walk into the room. Your chart is pre-populated. The head to toe starts with context, not data entry, and you catch things in the first minute that used to take 10.
How Sully.ai Supports Bedside Nurses
Sully is not one tool. It is a coordinated workforce of AI employees that share context and hand off cases: Scribe, Triage Nurse, Receptionist, and Coder. For every physician seeing patients, there are 10 administrative staff behind them, and each Sully AI role runs at 80 to 90% less than the cost of the equivalent human role.
Sully already supports 5,000+ providers and has delivered 50M+ hours of AI work across multiple specialties. See how Sully’s AI workforce removes documentation from the bedside and lets the nurse stay with the patient.
FAQ
Q: What is the correct order for a head-to-toe assessment?
The standard order is top down: general survey and vitals, then head and face, HEENT, neck, chest (heart and lungs), abdomen, extremities, skin, and neurological or musculoskeletal function. The one exception is the abdomen, where you auscultate before palpating so you do not alter bowel sounds. Running the same order every time is what prevents missed findings.
Q: How long does a head-to-toe assessment take?
A routine shift assessment on a stable patient takes about 10 to 15 minutes once you are proficient. A complete admission assessment runs 25 to 30 minutes because it includes full history, medication reconciliation, and detailed system reviews. Expect your first several exams in school or orientation to take longer while you build muscle memory for the sequence.
Q: What equipment do I need for a head-to-toe assessment?
At minimum: stethoscope, penlight, thermometer, blood pressure cuff, pulse oximeter, watch with a second hand, gloves, and hand sanitizer. A full kit adds a reflex hammer, tuning fork, tongue depressor, tape measure, and Snellen chart for vision screening. Most hospitals stock these at the bedside or on the medication cart.
Q: When should a nurse perform a head-to-toe assessment?
Nurses run a head to toe on admission, at the start of every shift, any time the patient’s condition changes, and before and after procedures. In critical care, abbreviated assessments happen every one to two hours. The goal is to set a baseline early so any deviation later in the shift is easy to catch.
Q: Can AI help with head-to-toe assessment documentation?
Yes. AI scribes like Sully.ai’s AI Scribe capture the assessment as you narrate it and populate the EHR in real time, which removes most end-of-shift charting. Sully’s AI Triage Nurse also collects pre-visit symptoms and history, so the head to toe starts with a pre-filled chart. Together they give back one to two hours of direct patient care time per shift.
TABLE OF CONTENTS
Hire your
Medical AI Team
Take a look at our Medical AI Team
AI Receptionist
Manages patient scheduling, communications, and front-desk operations across all channels.
AI Scribe
Documents clinical encounters and maintains accurate EHR/EMR records in real-time.
AI Medical Coder
Assigns and validates medical codes to ensure accurate billing and regulatory compliance.
AI Nurse
Assesses patient urgency and coordinates appropriate care pathways based on clinical needs.