If your contact center is still routing every refill call and appointment reschedule through a human agent, you are spending tens of millions of dollars a year to do work an AI agent can finish in 90 seconds.
Patient access is where most health systems quietly lose money and patient trust. Hold times stretch past five minutes, abandonment rates creep up, and scheduling lines go dark at 5 p.m. while patients need answers at 9 p.m. Healthcare contact center automation fixes that gap.
This guide walks through what automation actually is in 2026, which patient calls to automate first, the top vendors, how to roll it out, and the HIPAA guardrails you need before a single voice agent touches a live call.
The State of Patient Access in Healthcare Contact Centers
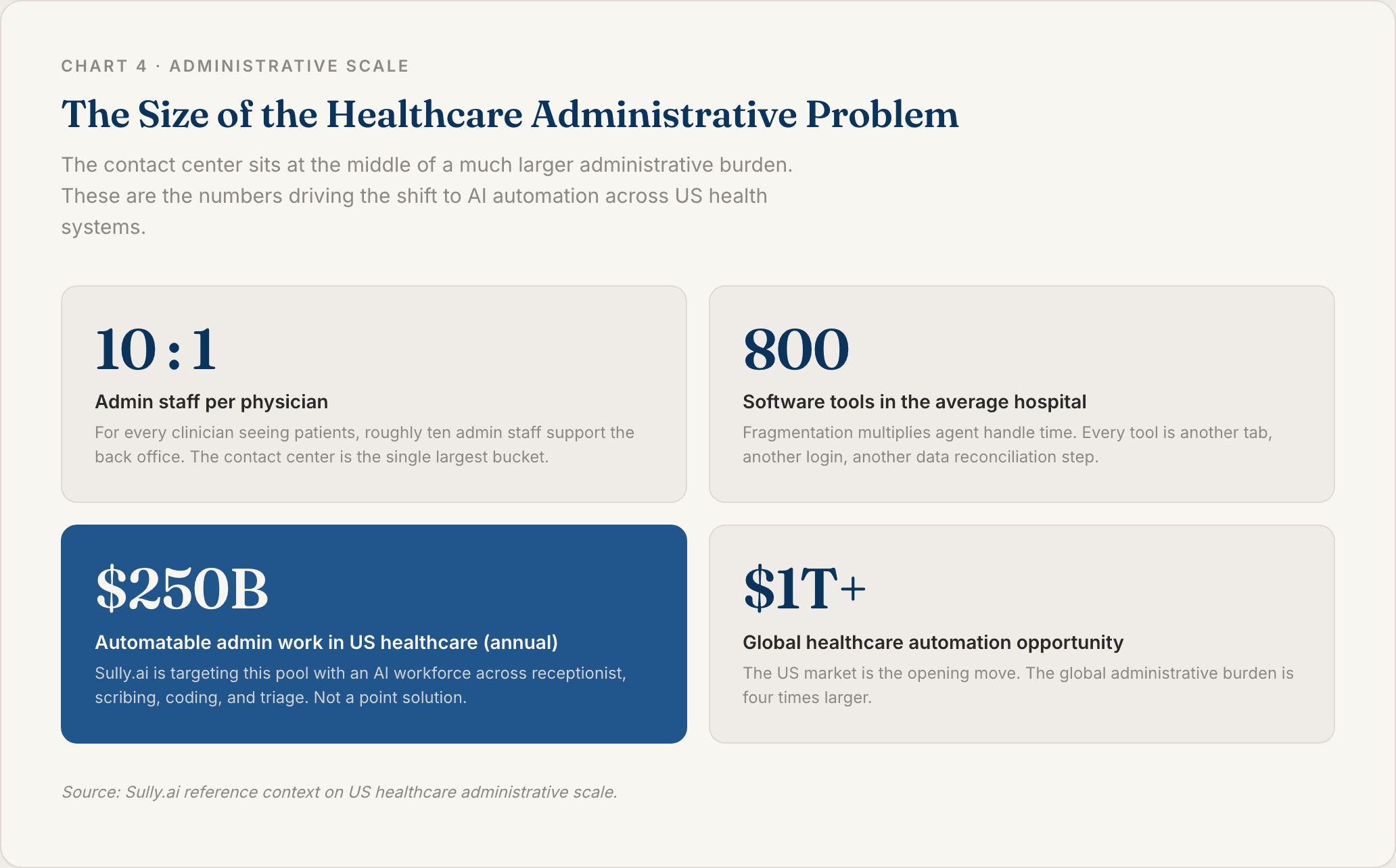
Here is something most health system CFOs do not realize. For every physician seeing patients, there are about 10 administrative staff behind them. A large share of that headcount sits in the contact center, answering the same questions day after day.
The average US hospital runs on 800 different software tools. Scheduling, EHR, billing, insurance verification, pharmacy, patient messaging. Every one of those systems touches the contact center. Agents toggle between five or six screens on a single call.
The numbers around this are big. The US healthcare industry has roughly $250 billion in automatable administrative work every year, and the global opportunity is over $1 trillion. A meaningful chunk of that sits inside the contact center.

Meanwhile patient expectations have shifted. Patients want the same experience they get from their bank or their airline: answers at any hour, across voice, text, chat, and web. Traditional call centers were never built for that.
What Healthcare Contact Center Automation Means Today
Healthcare contact center automation uses AI agents, voice bots, natural language processing, and workflow automation to resolve patient interactions end to end. Scheduling, refills, insurance checks, billing questions, and pre-visit intake. All without a human agent on the line for routine cases.
The goal is not to deflect patients. The goal is to finish the interaction. A patient calls to reschedule a visit. The AI agent verifies identity, checks the provider's calendar inside the EHR, books the slot, and texts a confirmation. Done.
How It Differs From Traditional Call Center Software
Legacy contact center stacks route calls. Modern healthcare automation resolves them.
Old IVR trees push patients through "press 2 for billing" menus and then dump them in a queue. A modern voice AI listens to "I need to refill my lisinopril," verifies the patient, checks refill eligibility in the EHR, and sends the script to the pharmacy. No menus.
The other big shift is deployment speed. A typical enterprise call center vendor takes 12 to 18 months to evaluate plus another 6 to 12 months to integrate with the EHR. That timeline is why most health systems have stalled on modernization. Newer platforms compress this into weeks, not quarters.
Core Components of an Automated Healthcare Contact Center
Five building blocks sit inside every modern deployment:
Conversational voice AI that handles natural spoken requests across accents and speech patterns
Omnichannel routing across voice, SMS, chat, email, and web so patients can start a conversation anywhere and finish it anywhere
EHR and CRM connectors that read and write appointment, demographic, and clinical data
HIPAA-compliant infrastructure with encryption at rest and in transit, plus full audit trails
Human handoff logic that knows when to escalate a clinical, financial, or emotional interaction
Point solutions usually cover one or two of these. A platform approach covers all five.
Where AI Agents Fit Into the Patient Journey
AI agents show up before, during, and after the visit. Pre-visit: they schedule, remind, collect intake, and verify insurance. During the visit: they document the encounter and triage follow-up calls. After the visit: they book follow-ups, coordinate refills, and resolve billing questions.
The strongest deployments let these agents hand off to each other. A doctor says "schedule a follow-up" at the end of a visit. The scribe captures it. The receptionist agent texts the patient. The appointment is on the books before the doctor finishes the next encounter.
Why Healthcare Contact Centers Are Under Pressure
Three forces are hitting at once: volume is up, labor is tight, and the tech stack is fragmented.
Rising Call Volumes and Staffing Shortages
Contact center agent turnover in healthcare commonly runs 30 to 45% a year. Every vacancy adds to hold times for the patients still on the line. Hiring and training replacements runs $5,000 to $7,500 per seat before the first call gets answered.
The 10 to 1 admin-to-physician ratio is not going to shrink by hiring harder. It shrinks by automating the work those admins spend their day on.
The Cost of Long Hold Times on Patient Satisfaction
Patients who wait on hold for more than two minutes abandon the call in large numbers. Those abandoned calls show up later as no-shows, missed refills, and negative HCAHPS scores. In some markets they show up as patient leakage to a competing health system.
Long hold times are not a service problem. They are a revenue problem.
Administrative Overhead From Fragmented Systems
Back to the 800 tools. A single scheduling call can touch the EHR, the practice management system, the insurance portal, and the patient messaging platform. An agent spends as much time hunting through tabs as talking to the patient.
Automation that sits across all of those systems, reading and writing in real time, is what finally closes the gap.
Benefits of Contact Center Automation in Healthcare
This is the section your CFO wants.
Reduced Call Handling Costs
A fully loaded contact center agent costs $45,000 to $60,000 per year in salary, benefits, management overhead, and training. An AI agent handling the same call volume runs 80 to 90% less than the human equivalent at Sully.ai pricing.
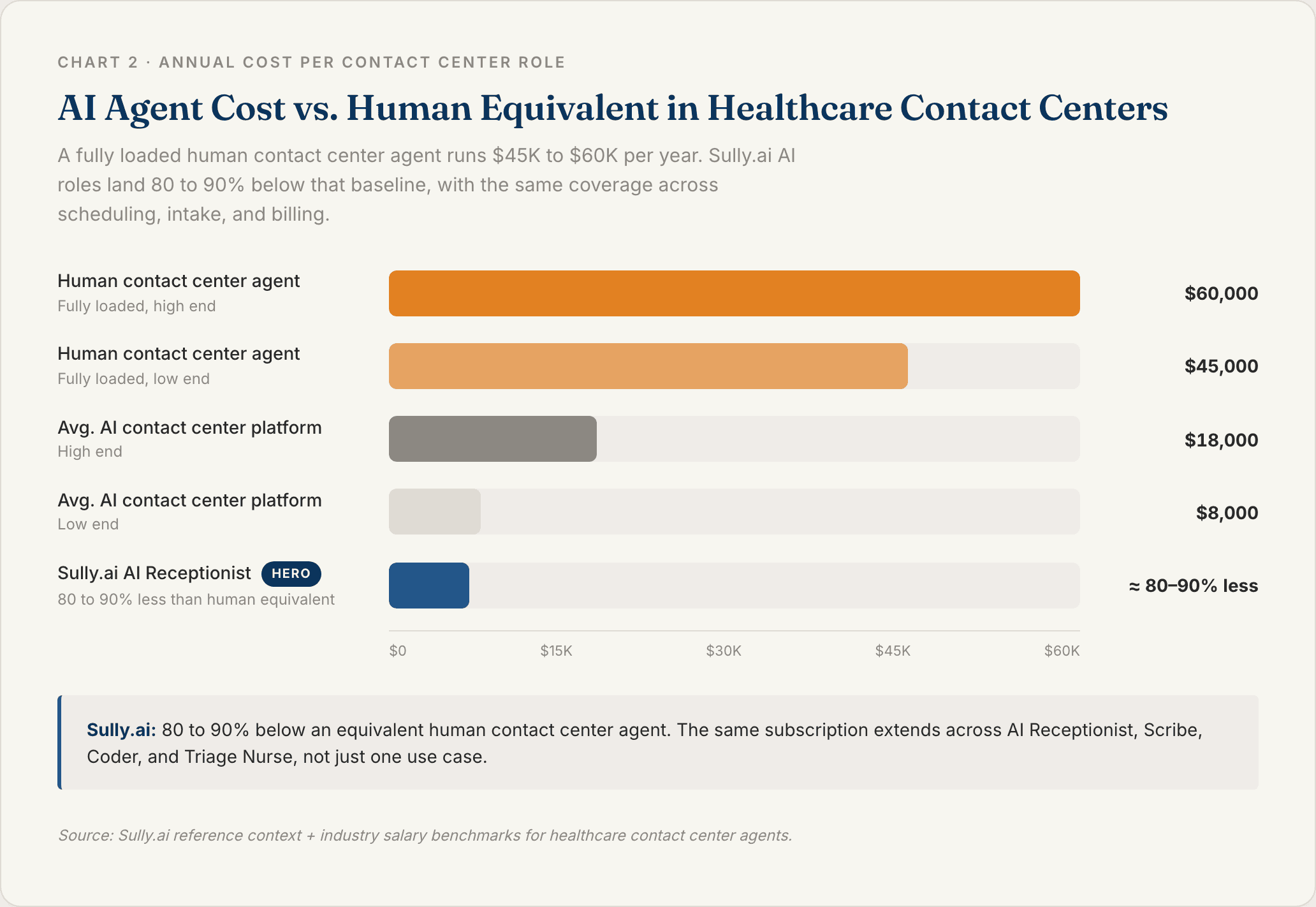
For a health system with 200 contact center FTEs, that math ends up in the eight figures annually. The savings compound because you stop paying turnover costs on the calls the AI now handles.
Around the Clock Patient Access
AI agents do not take shifts, vacations, or sick days. Patients can schedule at 10 p.m. on a Sunday and have a confirmed appointment before they go to bed. For health systems serving shift workers, caregivers, and rural populations, after-hours coverage is a real access win.
Fewer No Shows and Cancellations
Automated SMS and voice reminders, combined with one-tap rescheduling through the same channel, typically cut no-show rates in half. Baseline no-show rates sit around 15 to 30% across most specialties, so the reduction translates directly to filled schedules and captured revenue.
Higher Agent Retention and Lower Burnout
When AI handles the repetitive 80%, the refill calls, the reminder calls, the "what are your hours" calls, human agents get the complex 20%. The 20% is the work agents actually trained for: empathetic conversations, clinical triage nuance, and complex billing disputes.
Agents who spend their day on meaningful work quit less often.
Use Cases Across the Patient Journey
These are the workflows to automate, in rough order of ROI.
Automated Appointment Scheduling and Reminders
The single highest-volume use case. Voice AI takes new and existing patients through scheduling in natural language, checks provider availability against the EHR, books the slot, and sends an SMS confirmation. Reminders go out 72 and 24 hours before the visit with one-tap reschedule links.
Prescription Refill and Pharmacy Requests
Patients call or text requesting refills. The AI verifies identity, checks last fill date and refill eligibility against the EHR, routes to the prescriber only when approval is needed, and sends the script to pharmacy. Most refill requests never touch a human.
Insurance Verification and Prior Authorization
This is the outbound side of the contact center. AI agents call payers, sit through the on-hold music, navigate the IVR tree, verify eligibility, pull benefits, and flag prior-auth requirements. This is where voice AI saves the most agent hours, because payer calls routinely run 15 to 30 minutes each.
Pre Visit Intake and Symptom Triage
Before the visit, an AI triage nurse collects chief complaint, history of present illness, medications, allergies, and social history. The data lands in the chart before the doctor walks into the room. The physician opens a complete chart and starts the encounter on minute zero, not minute seven.
Billing, Claims, and Payment Inquiries
"What do I owe and why" is one of the most common call drivers. AI pulls the statement, explains the line items in plain English, takes a payment, or sets up a plan. Billing queues drop sharply, and collection rates go up because patients who understand the bill actually pay it.
Top Healthcare Contact Center Automation Companies
The vendor landscape splits into three groups. Healthcare-specific platforms, horizontal voice AI applied to healthcare, and legacy CCaaS platforms bolting AI on top.
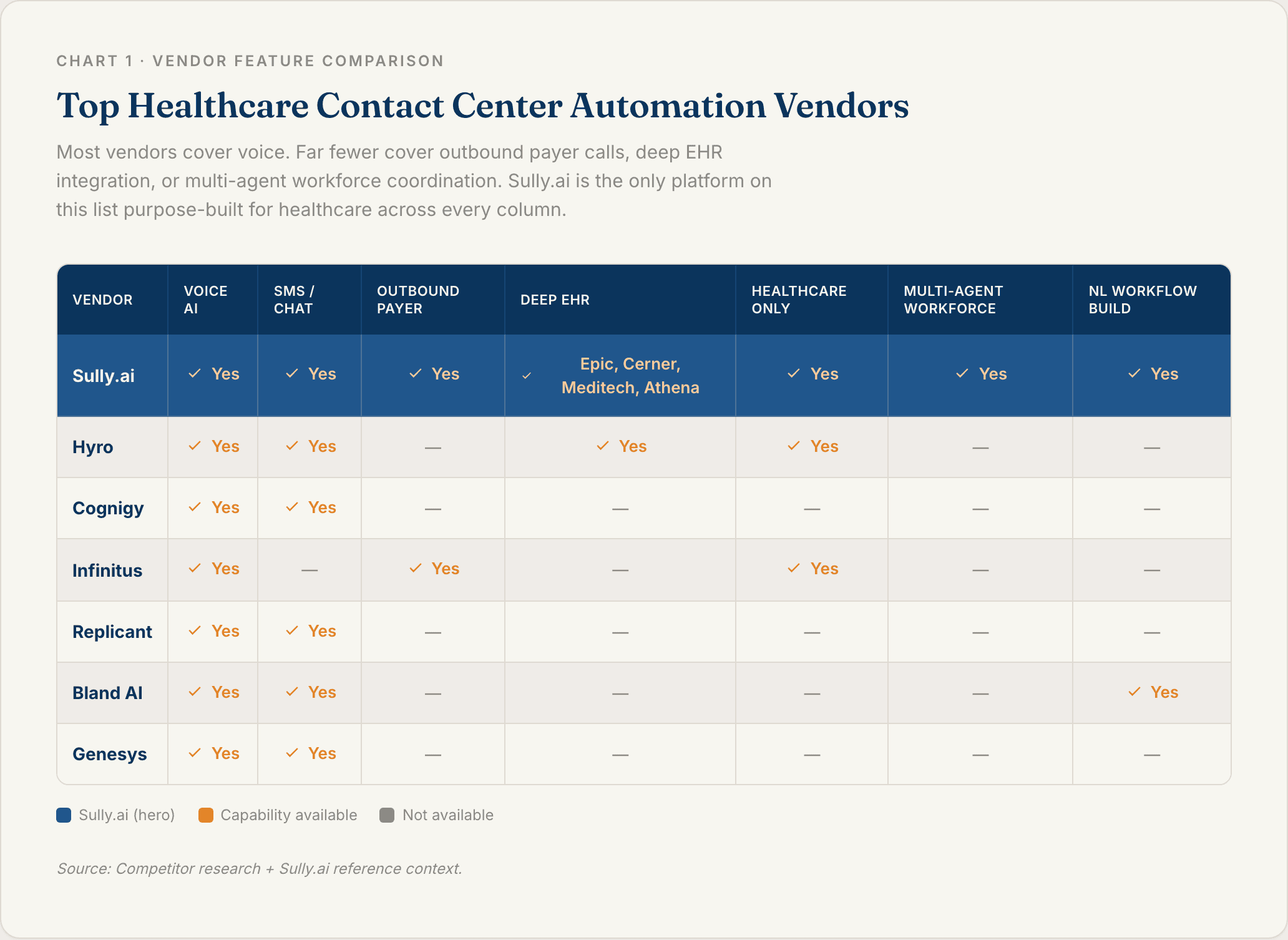
1. Sully.ai
Sully.ai is the only AI workforce built specifically for healthcare. Rather than selling a single AI tool, Sully deploys a coordinated team of AI employees: AI Receptionist, AI Scribe, AI Coder, AI Triage Nurse, and AI Consultant. Each has a defined role. Together they cover the full patient-access and revenue cycle.
The contact center angle runs through the AI Receptionist, but the real unlock is that the receptionist shares context with the scribe, coder, and triage agents. A scheduling call that produces new symptom information flows into the triage agent. A billing dispute flags a coding review.
Sully operates across 5,000+ providers and has delivered over 50 million hours of AI work. One integration covers Epic, Cerner, Meditech, and Athenahealth. Natural language customization lets an operations lead describe a workflow in plain English and have Sully assemble it, without a six-month engineering build.
Best for: health systems and large practice groups that want one vendor across contact center, documentation, coding, and patient outreach.
2. Hyro
Hyro is a conversational AI platform focused on healthcare call centers. The company positions around automating a high share of routine patient calls and offers both voice and chat channels. Strong fit for organizations that need a voice-first deployment without a full workforce platform.
3. Cognigy
Cognigy is an enterprise conversational AI platform serving multiple industries, including healthcare. Strengths are omnichannel coverage and multilingual support. Good option for multinational health systems or payers that need more than English-only voice.
4. Infinitus
Infinitus is a voice AI company specialized in outbound payer calls. Eligibility verification, benefits checks, and prior authorization are the core use cases. Teams that are drowning in payer hold time queues often start here before expanding into patient-facing calls.
5. Replicant
Replicant is a horizontal AI contact center platform with a healthcare industry vertical. Focuses on voice call automation and positions on "autonomous contact center" resolution.
6. Bland AI
Bland is a developer-friendly voice AI platform with a multi-modal healthcare offering across voice, SMS, and chat. Appeals to engineering teams that want to build custom workflows on top of an API rather than buy a pre-built product.
7. Genesys
Genesys is an incumbent contact center platform layering AI on top of an established CCaaS stack. Good fit for health systems already running on Genesys Cloud that want to add automation without ripping out the underlying phone system.
How to Implement Healthcare Contact Center Automation
A five-step rollout that does not blow up patient experience.
1. Map High Volume Patient Call Drivers
Pull 90 days of call data. Bucket by reason: scheduling, refills, billing, insurance, clinical questions, other. The top three categories almost always cover 60 to 75% of total volume and are the automation targets.
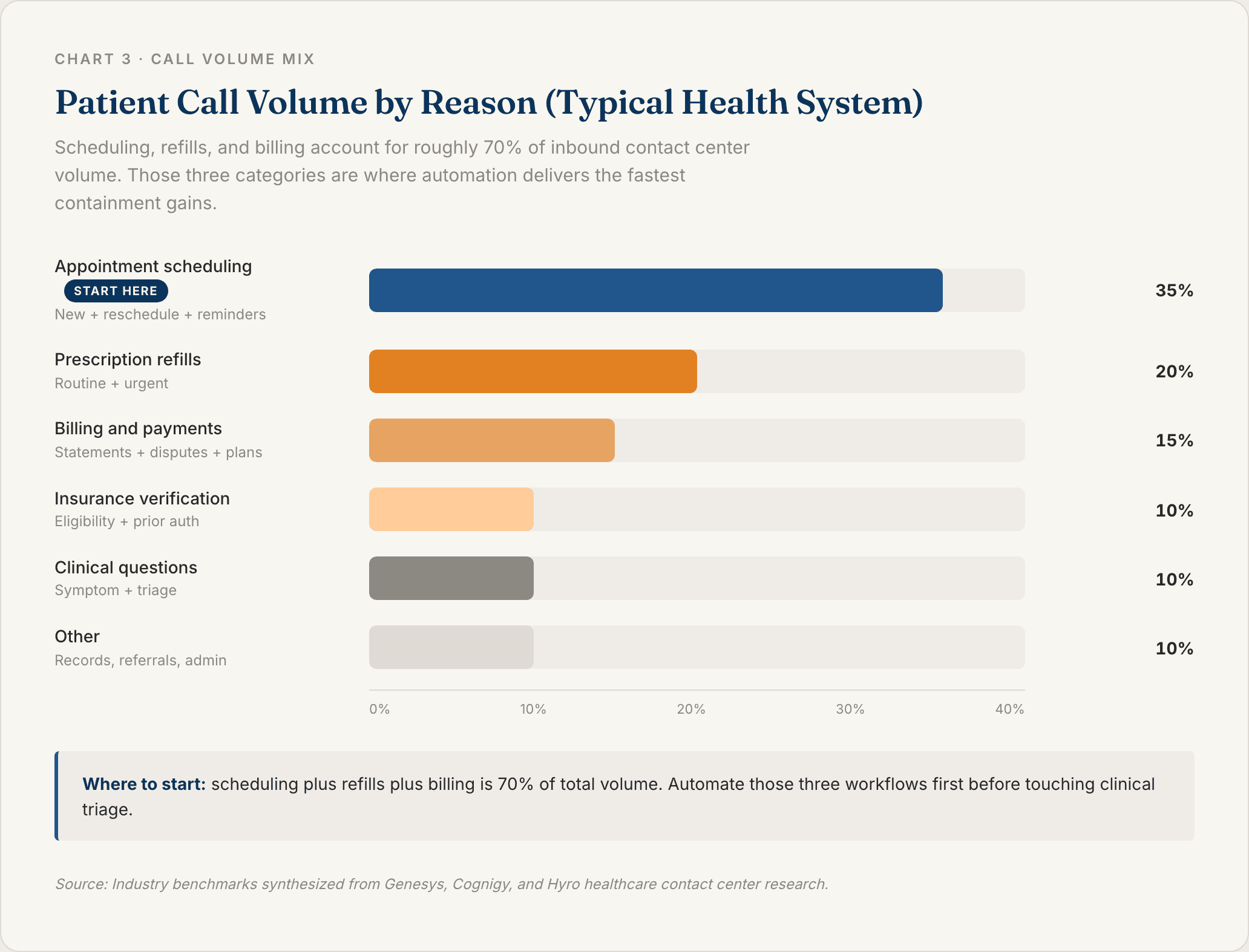
Do not start with whatever your vendor has the best demo for. Start with whatever eats the most agent hours.
2. Audit Your EHR and Telephony Stack
List every system the AI will need to read from and write to. EHR, scheduling, patient messaging, billing, telephony, payer portals. Identify integration gaps before you sign a vendor contract.
This is where single-integration platforms save months. If one vendor already connects to Epic, Cerner, Meditech, and Athena, you skip four separate integration projects.
3. Start With Automated Scheduling and FAQ Routing
Highest ROI, lowest clinical risk. Deploy the AI on appointment booking and FAQ containment before touching clinical triage. Measure containment rate week over week and only expand scope when containment is stable above 70% for the pilot workflows.
4. Define HIPAA Guardrails and Escalation Rules
Before go-live, document three things in writing:
Exactly what PHI the AI reads, stores, and transmits
Full logging and audit trail requirements
The precise conditions under which a call escalates to a human (clinical symptoms, payment disputes, detected emotional distress, explicit patient request)
A missing escalation rule is how a clinical automation failure becomes a news story.
5. Measure Containment Rate and Patient Satisfaction
Two metrics matter most. Containment rate is the percent of calls fully resolved by the AI without a human handoff. Patient CSAT or NPS on automated interactions tells you whether the AI is actually resolving the issue or just deflecting it.
If containment is rising but CSAT is falling, the AI is kicking patients off the phone without finishing the job. Fix it before scaling.
Security, HIPAA, and Compliance Considerations for Healthcare Automations
Contact center automation runs on PHI. Which means it runs under HIPAA. Which means your security and legal teams get a vote before the vendor gets a signature.
Protected Health Information Handling
Ask every vendor four questions and get written answers:
Where is PHI encrypted (at rest, in transit)
Where are voice recordings and transcripts stored, and for how long
What data minimization controls are in place
Which subprocessors touch the data
"Our platform is HIPAA compliant" is marketing copy. The four answers above are what actually matters.
Audit Trails and Call Recording Rules
Every AI-handled interaction should be logged with timestamps, inputs, AI decisions, and outcomes. You need this for HIPAA audits. You also need it to debug model behavior when an agent answers something incorrectly.
State recording laws still apply. Two-party consent states require disclosure even when the "party" is an AI.
Vendor Risk and BAA Requirements
Any vendor handling PHI must sign a Business Associate Agreement. The BAA should name subprocessors, specify data residency, and include a breach notification timeline that matches or beats the HIPAA 60-day requirement. If the vendor resists naming subprocessors, walk away.
Unifying Healthcare Contact Centers With the Sully.ai AI Workforce
Most AI vendors built tools. Each one solves one problem. None of them talk to each other. Sully built a workforce. AI employees that share context, hand off cases, and work as a team across the full patient journey.
That distinction matters most in the contact center, because a call is rarely about one thing.
Coordinated AI Agents Across Scheduling, Scribing, and Coding
A real patient interaction at a Sully customer looks like this:
Patient calls to reschedule. AI Receptionist books the new slot.
The same patient mentions a new symptom. AI Triage Nurse collects structured history and flags it for the physician.
The prior visit note from AI Scribe already contains the clinical context the nurse needs.
After the next visit, AI Coder extracts the ICD-10 and CPT codes and submits a clean claim before a denial can happen.
Four agents. One patient. Zero handoffs lost because the context flows between them automatically.
Single EHR Integration Across Epic, Cerner, and Athenahealth
One integration covers every agent. Sully connects once to the EHR and every AI employee reads from the same data. Most vendors in this space require a separate integration project per deployment, which is how 6 to 12 month timelines become 18 month timelines.
Natural Language Workflow Customization
Describe the workflow in plain English. "When a patient misses an appointment, call them within 24 hours, offer a rebook, and if they do not answer, text them a booking link." Sully assembles the workflow. No custom engineering. No separate vendor implementation team.
For a contact center operations lead, that means you ship changes in days, not quarters.
FAQ
Q: What is healthcare contact center automation?
Healthcare contact center automation uses AI agents, voice bots, and workflow automation to resolve patient interactions across voice, SMS, and chat channels without a human agent for routine requests. It covers scheduling, refills, insurance, billing, and pre-visit intake. Modern platforms like Sully.ai extend this into an AI workforce where receptionist, scribe, coder, and triage agents share context across the full patient journey.
Q: How is healthcare call center automation different from contact center automation?
The terms often get used interchangeably. In practice, "call center" typically refers to voice-only operations while "contact center" spans voice, SMS, chat, email, and web. Healthcare contact center automation is the broader category and is where modern AI platforms operate, because patients reach providers across every channel.
Q: How much do healthcare automation companies typically charge?
Pricing varies by call volume, channels, and integration scope. Most vendors price per minute of AI voice time, per conversation, or as an enterprise subscription tied to patient volume. Each Sully.ai AI role costs 80 to 90% less than the equivalent human headcount, which is a useful baseline when comparing vendor quotes.
Q: What patient calls should be automated first?
Start with scheduling, appointment reminders, and FAQ deflection. Those workflows cover the largest share of total contact center volume, carry the lowest clinical risk, and show measurable containment gains within weeks. Expand into refills, insurance verification, and pre-visit intake once guardrails and escalation paths are proven.
Q: How does Sully.ai handle healthcare contact center workflows?
Sully.ai deploys a team of AI employees (Receptionist, Scribe, Coder, Triage Nurse, and Consultant) that share context and hand off cases across the patient journey. Unlike point-solution vendors that require separate integrations per tool, Sully integrates once with Epic, Cerner, Meditech, or Athenahealth and operates across scheduling, documentation, coding, and patient outreach as a coordinated workforce.
TABLE OF CONTENTS
Hire your
Medical AI Team
Take a look at our Medical AI Team
AI Receptionist
Manages patient scheduling, communications, and front-desk operations across all channels.
AI Scribe
Documents clinical encounters and maintains accurate EHR/EMR records in real-time.
AI Medical Coder
Assigns and validates medical codes to ensure accurate billing and regulatory compliance.
AI Nurse
Assesses patient urgency and coordinates appropriate care pathways based on clinical needs.