HPI stands for History of Present Illness. It’s the narrative section of a medical record where a clinician describes the patient’s current health concern in chronological detail, covering eight elements defined by CMS.
If you’ve ever seen “HPI” in a SOAP note, a chart audit, or a billing denial, that’s what it means. The HPI is the story behind the chief complaint, and its depth directly controls the billable level of the visit.
This guide covers what HPI stands for, the eight required elements, how Brief and Extended HPI affect E/M coding, how to write a strong one, and how AI scribes like Sully.ai capture the whole thing automatically.
What HPI Stands For in Medical Records
HPI is short for History of Present Illness. In the UK, the same section is called the History of Presenting Complaint (HPC), but the structure is identical.
The HPI sits right after the chief complaint in a clinical note. The chief complaint is the one-line reason the patient came in. The HPI is the detailed story that follows.
It’s easy to confuse HPI with the rest of a patient’s history. Keep these separate:
Chief Complaint (CC): one-line reason for the visit
HPI: chronological narrative of the current concern
ROS: head-to-toe symptom review
PMH / PFSH: past medical, family, and social history
The CMS 1995 and 1997 Documentation Guidelines are the source of truth for what counts as a compliant HPI. Every auditor, biller, and coder pulls from the same playbook.
The 8 Elements of an HPI
CMS defines eight HPI elements. The number of elements documented is what separates a Brief HPI from an Extended HPI, and it’s the single biggest driver of E/M level on the history side.
Here’s the quick reference.

Location
Where on the body the symptom is happening. “Chest pain” is weak. “Substernal chest pain radiating to the left arm” is strong.
Quality
The character of the symptom. Sharp, dull, burning, crushing, throbbing. This is how a patient describes what it feels like.
Severity
A number on a 0–10 scale, or a comparison (“worst headache of my life”). Severity is the element most often missed, and it’s required for an Extended HPI.
Duration
How long the symptom has been present. “Three days” is duration. “Started three days ago” is duration plus onset.
Timing
When during the day or in what pattern the symptom occurs. Morning, nocturnal, post-meal, intermittent every 20 minutes.
Context
What the patient was doing when it started or what situation brings it on. After meals, during exercise, at rest, after medication changes.
Modifying Factors
What makes the symptom better or worse. Rest, ice, NSAIDs, position change, food. This is where clinical reasoning starts to come through.
Associated Signs and Symptoms
What else is showing up at the same time. Nausea with chest pain. Photophobia with headache. Dyspnea with fatigue. These are the clues that move the differential.
Brief HPI vs Extended HPI
CMS splits the HPI into two tiers, and the tier you document caps your E/M level.
Brief HPI: 1 to 3 elements
Extended HPI: 4 or more elements, OR the status of 3 or more chronic or inactive conditions

How Brief HPI Affects E/M Level
A Brief HPI caps the visit at Expanded Problem Focused for established patients. That’s an E/M level 3, and the reimbursement difference between a level 3 and a level 4 visit can be 40–60% per encounter.
If you’re documenting three elements when the visit actually warranted five, you’re leaving money on the table every single day.
How Extended HPI Affects E/M Level
An Extended HPI unlocks Detailed and Comprehensive history, which supports E/M level 4 and 5. The 1997 guidelines added an alternative path: documenting the current status of three or more chronic conditions counts as Extended.
That alternative matters for primary care and chronic care management, where patients often come in with a short current complaint but several ongoing problems.
Why HPI Matters for Clinical Documentation
The HPI is doing three jobs at once. It drives diagnosis, it sets the billing level, and it protects you in an audit or a lawsuit.
Impact on Diagnostic Accuracy
The HPI is where the differential gets built. A specific, structured narrative narrows the possibilities before a single test gets ordered.
Vague HPIs push clinicians toward over-testing. Specific HPIs do the opposite. Less imaging, fewer labs, faster answers.
Impact on Billing and E/M Coding
Under-documented HPIs are the number one reason for E/M downcoding on audit. Payers look at the elements, count them, and decide whether the visit level was justified.
A note that describes severity, timing, and modifying factors in one sentence passes. A note that just says “patient reports pain” does not.
Impact on Legal and Audit Defense
In a malpractice case, the HPI is the record of what the patient told you and what you thought about it. A thin HPI is indefensible.
Copy-forward HPIs are worse. If last week’s HPI shows up in this week’s note word-for-word, an auditor will assume the exam never happened.
How to Write a Strong HPI
Two habits separate strong HPIs from weak ones: using a mnemonic and writing in focused narrative.
OLD CARTS and OPQRST Mnemonics
Both mnemonics cover the eight CMS elements with different mental models. Pick the one that sticks.
OLD CARTS | OPQRST |
|---|---|
Onset | Onset |
Location | Provocation / palliation |
Duration | Quality |
Character | Radiation |
Aggravating / alleviating | Severity |
Radiation | Timing |
Timing | |
Severity |
OLD CARTS is more common in primary care and internal medicine. OPQRST is the emergency and EMS standard. Either one works.
Narrative Format and SOAP Integration
The HPI lives in the “S” of a SOAP note. Write it as a paragraph, not a list.
“Mr. K is a 58-year-old with substernal chest pressure that started 30 minutes ago while climbing stairs. Pain is 7/10, dull and squeezing, radiating to the left arm, associated with nausea and diaphoresis. Relieved partially by rest. No prior episodes.”
That’s six elements in four sentences: location, quality, severity, duration, timing, context, modifying factors, associated symptoms. Extended HPI, E/M level 4 or 5 eligible.
Common HPI Documentation Mistakes
Missing severity (the most commonly skipped element)
No timeline or onset
Vague modifying factors (“nothing helps”)
Copy-forward from prior notes
Mixing HPI with ROS (“no fever, no chills, no headache” belongs in ROS)
Fix those five and the quality of your notes lifts immediately.
HPI Documentation Challenges in the EHR Era
HPI quality is falling in most health systems, and the EHR is the main reason.
Time Burden on Physicians
Physicians spend roughly two hours on documentation for every hour of patient care. The HPI is one of the most text-heavy fields in the note, and typing it while talking to a patient is where most of that time goes.
Copy-Forward and Note Bloat
Copy-forward was supposed to save time. It created a second problem: charts full of inaccurate, repeated narratives that don’t reflect the current visit.
Auditors flag copy-forwarded HPIs routinely. Some payers now deny claims when the HPI from consecutive visits is identical.
Template Rigidity and Missed Nuance
Structured templates and dropdowns were supposed to fix note bloat. Instead, they stripped out the narrative thread that makes an HPI clinically useful.
A dropdown for “quality = sharp” loses the patient’s actual words. Words matter in medicine. Templates can’t carry them.
How AI Scribes Automate HPI Documentation
Ambient AI scribes record the visit, extract each HPI element, and write the narrative into the EHR before the physician leaves the room.
Sully.ai is an AI workforce built specifically for healthcare. Sully’s AI Scribe listens to the conversation and produces a full HPI. Sully’s AI Coder reads that HPI and pulls the ICD-10 and CPT codes. The claim goes out clean.
Capturing the 8 HPI Elements Automatically
Sully’s AI Scribe is trained to structure its output around the CMS elements. Location, quality, severity, duration, timing, context, modifying factors, associated symptoms. Every visit, no dropdowns, no templates.
The narrative comes out in the physician’s voice, not in stock template language.
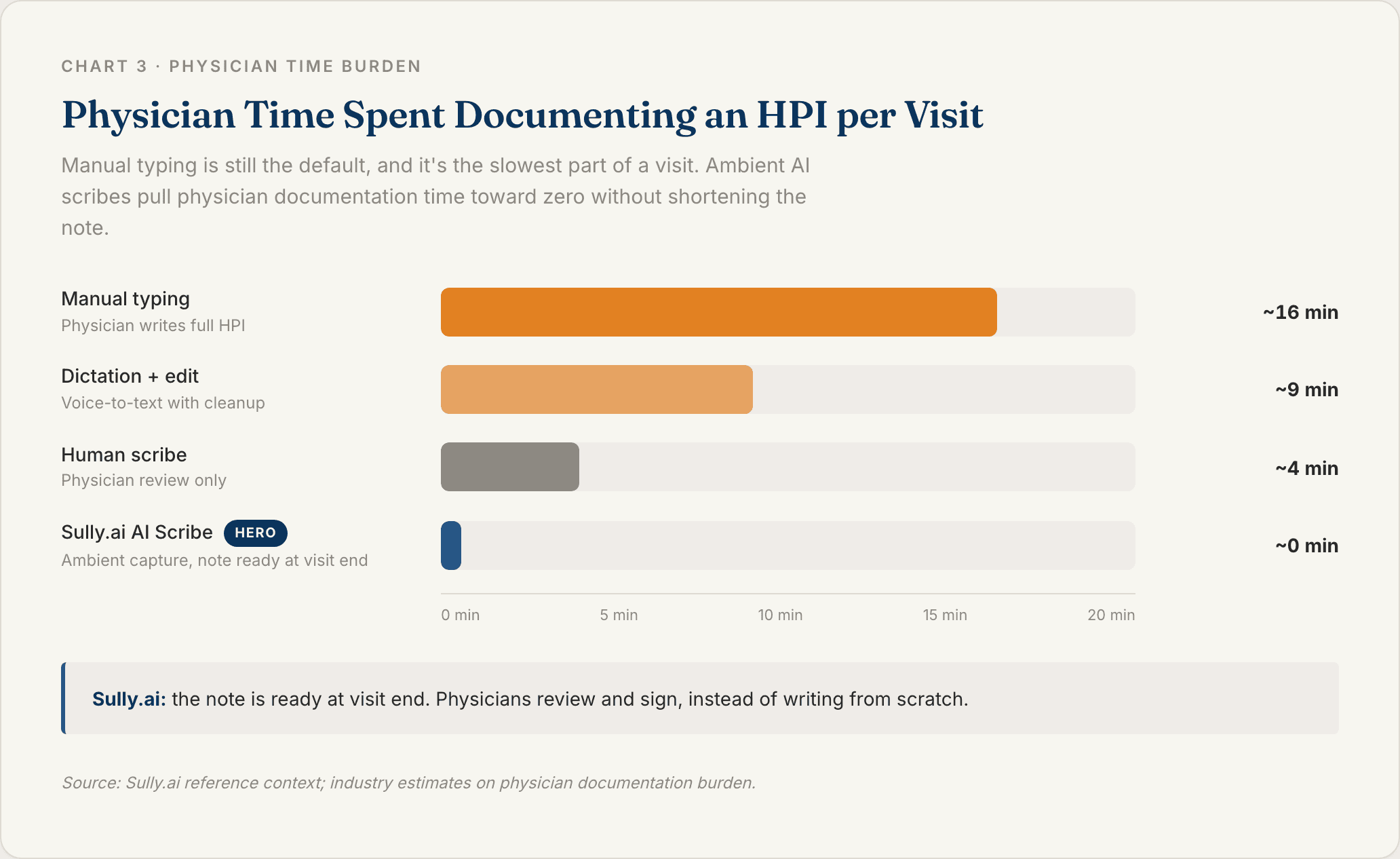
Chart 3: HPI Documentation Time by Method
Connecting HPI to Coding and Billing
This is where most AI scribes stop. Sully does not.
The AI Scribe hands the finished HPI to the AI Coder. The Coder extracts ICD-10 and CPT codes, checks them against payer rules, and submits a clean claim. An Extended HPI gets coded as an Extended HPI, automatically.
That handoff is the difference between a note that exists and a note that gets paid.
Cutting Documentation Time Without Cutting Detail
Sully.ai serves 5,000+ providers and has delivered 50M+ hours of AI work. Each Sully AI role costs 80–90% less than the equivalent human role.
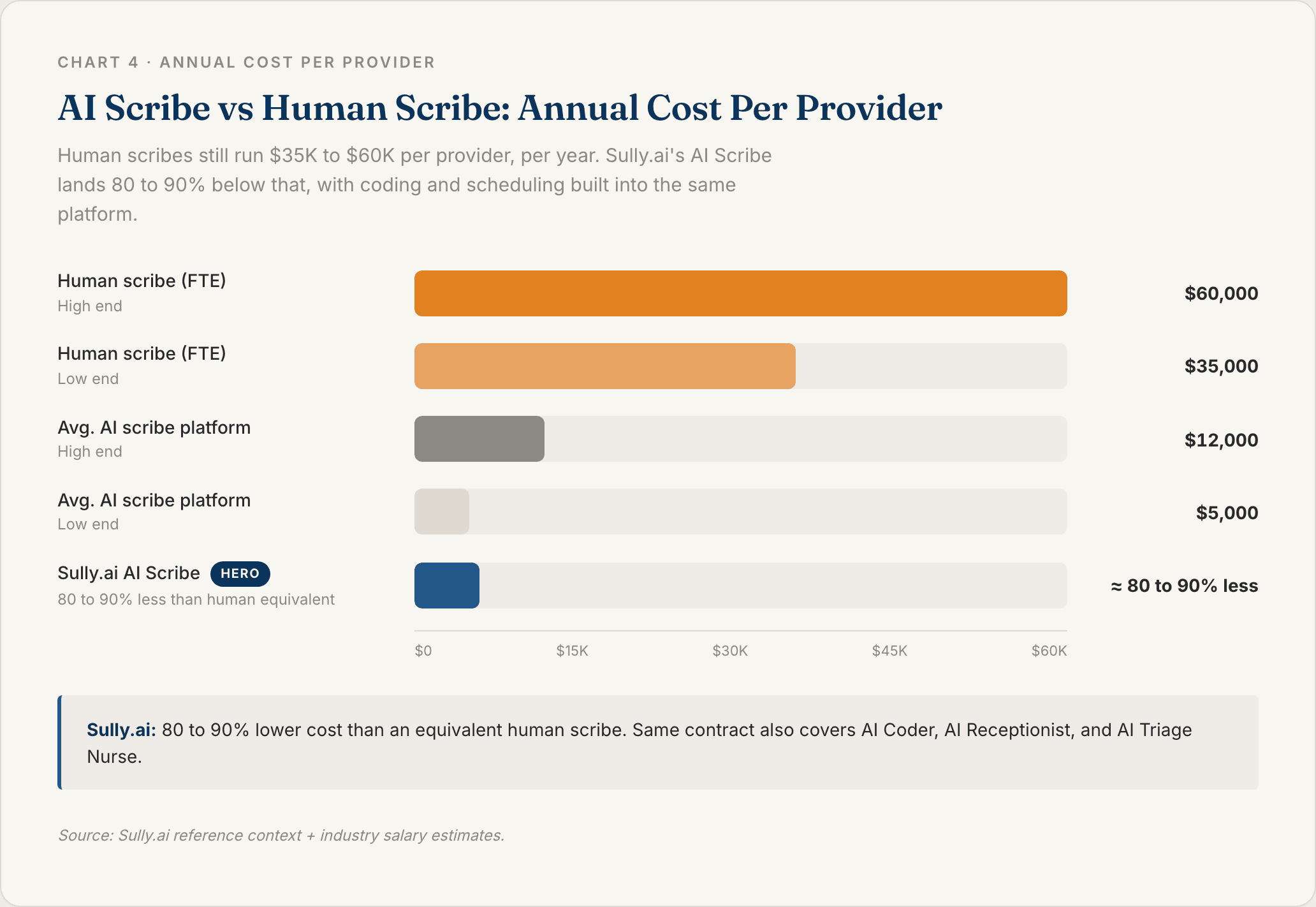
Chart 4: AI Scribe vs Human Scribe Annual Cost
Physicians using Sully reclaim hours per week. HPIs get more detailed, not less. That’s the pattern we see across specialties and EHRs (Epic, Cerner, Meditech, Athenahealth), all through a single integration.
FAQ
Q: What does HPI stand for in medical terms?
HPI stands for History of Present Illness. It’s the section of a medical record that narrates a patient’s current health concern in chronological detail, covering onset, location, quality, severity, timing, context, modifying factors, and associated symptoms. Every E/M visit note includes an HPI, and its depth directly determines the billable visit level. Sully.ai’s AI Scribe captures all eight HPI elements automatically during the patient visit.
Q: What are the 8 elements of an HPI?
The CMS 1995 and 1997 Documentation Guidelines define eight HPI elements: location, quality, severity, duration, timing, context, modifying factors, and associated signs and symptoms. A Brief HPI documents 1 to 3 elements and supports lower E/M levels. An Extended HPI documents 4 or more elements (or the status of 3+ chronic conditions) and supports Detailed or Comprehensive history levels.
Q: What is the difference between HPI and chief complaint?
The chief complaint (CC) is a one-line statement of why the patient came in, for example “chest pain for two hours.” The HPI is the full narrative that develops that complaint across the eight documented elements. Both appear in every E/M note, but the chief complaint is a headline while the HPI is the story.
Q: How long should an HPI be?
There is no minimum word count, but there is a minimum element count. A Brief HPI needs 1 to 3 elements. An Extended HPI needs 4 or more. In practice, well-documented HPIs are 3 to 6 sentences of focused narrative. Length for its own sake does not raise E/M level. Specificity does.
Q: Can AI write an HPI?
Yes. Ambient AI scribes like Sully.ai listen to the patient-physician conversation, identify each of the eight HPI elements, and write a complete narrative directly into the EHR. Sully.ai’s AI Scribe serves 5,000+ providers and cuts documentation time compared to typing HPIs manually or using a human scribe, at 80–90% lower cost than the human equivalent.
TABLE OF CONTENTS
Hire your
Medical AI Team
Take a look at our Medical AI Team
AI Receptionist
Manages patient scheduling, communications, and front-desk operations across all channels.
AI Scribe
Documents clinical encounters and maintains accurate EHR/EMR records in real-time.
AI Medical Coder
Assigns and validates medical codes to ensure accurate billing and regulatory compliance.
AI Nurse
Assesses patient urgency and coordinates appropriate care pathways based on clinical needs.