Documentation is quietly breaking American healthcare. Physicians today spend nearly 2 hours on paperwork and EHR tasks for every hour of direct patient care, according to Tebra's 2025 Physician Burnout Survey. This is a structural crisis driving 43.2% of U.S. physicians to report at least one symptom of burnout even as overall rates finally begin to decline.
AI medical scribes are emerging as one of the most practical, proven solutions to this problem. By listening to doctor-patient conversations and automatically generating structured clinical notes, these tools are giving clinicians back something irreplaceable: time with patients.
This complete guide covers everything you need to know, how AI medical scribes work, what features actually matter, how to evaluate your options, and what the latest research says about their real-world impact.
Key Takeaways
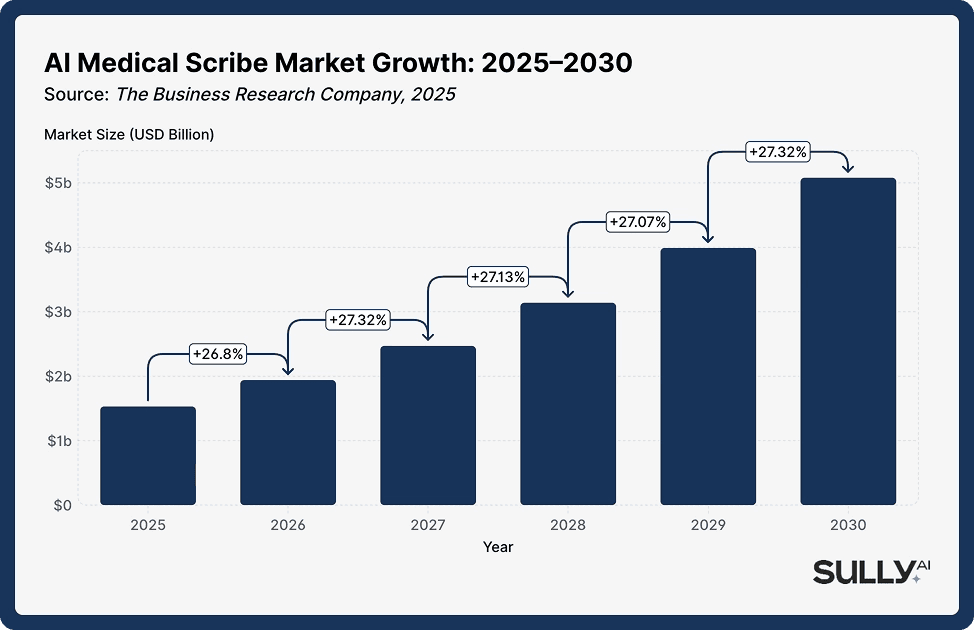
The market is exploding: The global AI medical scribe software market reached USD 1.53 billion in 2025 and is forecast to hit $5.08 billion by 2030, driven by rising physician burnout and EHR adoption.
Documentation is the #1 burnout driver: Administrative and documentation burden, not patient care, is consistently cited as the leading cause of physician burnout, with 68% of physicians reporting increased AI use for clinical documentation in 2024.
AI scribes deliver measurable relief: Ambient documentation tools reduced clinician burnout by 21.2% at Mass General Brigham and improved documentation-related well-being by 30.7% at Emory Healthcare, per a peer-reviewed JAMA Network Open study.
Adoption is accelerating fast: Major health systems including Kaiser Permanente, Cleveland Clinic, and UCSF Health have deployed AI scribing platforms enterprise-wide, with 65-70% of Kaiser Permanente physicians already using Abridge AI scribe tools.
Security and compliance are table stakes: The best AI scribe platforms are HIPAA-compliant by default, using end-to-end encryption, multi-factor authentication, and real-time anomaly detection to protect patient data.
What Is an AI Medical Scribe?
An AI medical scribe is a digital assistant that uses artificial intelligence, natural language processing (NLP), and machine learning to automatically document clinical encounters in real time. Sully the Scribe, for example, listens to doctor-patient conversations, filters for clinically relevant content, and generates a structured note, typically formatted for direct entry into an EHR system.
This is fundamentally different from traditional transcription software, which simply converts audio to text. AI medical scribes understand context. They know the difference between a patient mentioning a headache casually and a physician documenting a chief complaint. They apply clinical structure (SOAP notes, problem lists, assessment and plan sections) without requiring the physician to dictate explicitly.
Pro Tip: The best AI scribes don't just transcribe, they synthesize. A well-trained model can infer that a mention of "follow up in two weeks" should populate the plan section, not just appear as a sentence in the note. That contextual intelligence is what separates modern ambient scribes from older voice-to-text tools.
The core workflow is simple:
Clinician activates the scribe at the start of an encounter (usually via a smartphone or tablet app)
The AI listens to the ambient conversation using voice recognition
The system generates a draft note in real time or immediately after the visit
The clinician reviews and approves the note, making any edits before signing
The note is pushed to the EHR, completing documentation in minutes rather than hours
Sully's AI Scribe integrates directly with existing EHR and EMR systems, meaning notes land where they need to be without manual re-entry.
How AI Medical Scribes Work: The Technology Behind the Notes
Natural Language Processing and Machine Learning
At the core of every AI scribe is a combination of natural language processing (NLP) and machine learning. NLP allows the system to understand human speech, including medical jargon, abbreviations, and conversational shorthand. Machine learning enables continuous improvement: the more the system is used, the better it gets at understanding the preferences, phrasing patterns, and documentation style of each individual clinician. To go deeper on the technology, Sully's guide to AI scribe technology covers how these advances are reshaping medical documentation.
A 2024 study published in Computers in Human Behavior Reports found NLP technologies achieve over 70% precision in labeling symptoms, detecting emotions, and quantifying pain from medical records and patient self-reports, outperforming traditional documentation methods significantly.
Modern AI scribes also incorporate large language models (LLMs), the same underlying technology powering general-purpose AI assistants, but fine-tuned on clinical datasets. This allows them to interpret nuanced exchanges and organize them into the specific note formats used by different specialties.
Ambient Listening and Real-Time Documentation
Unlike older dictation tools that required physicians to speak directly into a device, modern AI scribes use ambient listening technology. The microphone captures the natural flow of conversation, including patient responses, clinician questions, and any back-and-forth, without interrupting the clinical encounter.
This is a fundamental shift in workflow. Rather than documenting after the visit (which is where most of that "pajama time" EHR work happens), ambient scribes generate notes during the encounter. Physicians can review a near-complete draft the moment the patient walks out the door.
Handling Accents, Dialects, and Medical Terminology
Healthcare is one of the most linguistically diverse industries in the world. Physicians, nurses, and patients come from hundreds of different linguistic backgrounds, and traditional transcription tools have historically struggled with non-standard accents and specialized terminology.
Modern AI scribes are trained on vast, diverse speech datasets that include global accents and regional dialects. Most leading platforms also support multilingual documentation, allowing encounters to be transcribed accurately regardless of the primary language spoken, a growing priority for health systems serving multicultural communities.
EHR Integration
AI scribes don't exist in isolation. Their value multiplies when they connect directly with electronic health record platforms. Seamless EHR integration means:
Notes populate the correct fields automatically (chief complaint, HPI, assessment & plan, etc.)
Patient demographics and prior history are accessible to the scribe for context
Billing codes and diagnoses can be suggested based on documented content
No duplicate data entry across systems
Sully connects with major EHR systems to ensure clinical notes land directly where they belong, accurately and without additional manual steps.
Key Features to Look for in AI Medical Scribe Software
Not all AI scribes are built the same. Here's what actually differentiates the best platforms from the rest:
Voice Recognition Accuracy and Speed
Accuracy is non-negotiable in clinical documentation. A misheard word can change a diagnosis code, affect reimbursement, or worse, compromise patient safety. Look for platforms that:
Achieve >95% transcription accuracy across multiple accents and dialects
Operate in real time (not post-processing with significant delay)
Handle medical terminology natively, including abbreviations like HTN, DM2, CABG, and thousands of specialty-specific terms
Adapt to individual clinician styles through continuous learning
Specialty-Specific Customization
Each medical specialty has unique documentation workflows. A psychiatry note looks entirely different from a surgery operative report or a pediatric well-child visit. Strong AI scribe platforms offer:
Pre-built templates for major specialties (internal medicine, family medicine, emergency medicine, psychiatry, surgery, etc.)
Customizable note structures per physician preference
The ability to include or exclude specific elements based on practice patterns
Intelligent suggestions for specialty-specific diagnoses and treatment plans
"One thing I've found is that customization options matter far more than most clinicians realize before implementation. A scribe that understands your specialty's documentation logic from day one cuts your review time dramatically compared to a generic one-size-fits-all tool."
Security, HIPAA Compliance, and Data Privacy
Patient data is among the most sensitive information that exists. HIPAA compliance is the baseline requirement, not a premium feature. When evaluating any AI scribe, verify:
End-to-end encryption for all audio and text data in transit and at rest
Multi-factor authentication (MFA) for all users
Real-time anomaly detection to flag unusual access patterns
Data retention and deletion policies that align with regulatory requirements
Business Associate Agreement (BAA) availability
Transparent consent processes for patients regarding data usage
The question of whether audio recordings are retained after notes are generated is particularly important, different platforms handle this differently, and it has meaningful privacy implications.
Billing and Coding Support
A significant, and often underappreciated, benefit of AI scribes is their impact on revenue cycle accuracy. When documentation is more complete and structured:
Billable diagnoses are less likely to be missed
Procedure and visit level codes are easier to assign accurately
Claim rejection rates decrease due to better supporting documentation
Audit risk decreases because notes consistently meet payer standards
Some platforms extend this further with dedicated AI coding tools that validate and assign codes automatically based on the clinical note content.
The Real Benefits of AI-Powered Medical Documentation
Reducing Administrative Burden and Reclaiming Clinical Time
The numbers are stark. More than one-third of physicians cite ineffective EHR systems, documentation requirements, and in-basket burden as a major source of job stress, work that frequently spills into evenings and weekends. The AMA has tracked a consistent pattern of physicians spending more time with computers than with patients.
AI scribes directly attack this problem. In real-world deployments:
Physicians using AI save an average of 12 minutes per visit, translating to roughly 2 hours per day in a typical primary care schedule
Ambient documentation tools reduced clinician burnout by 21.2% at Mass General Brigham in a peer-reviewed JAMA Network Open study
Documentation-related well-being improved by 30.7% at Emory Healthcare in the same study
93% of independent primary care physicians expect AI scribe tools to reduce documentation burden, with 89% anticipating better job satisfaction
The bottom line: when physicians aren't fighting their documentation systems, they have more cognitive and emotional bandwidth for the work they trained for.
Improving Documentation Accuracy and Consistency
Human documentation is inherently variable. When a physician is tired, rushed, or seeing their 25th patient of the day, notes get shorter, less precise, and more prone to omission. AI scribes don't experience fatigue.
These systems follow consistent documentation protocols every time, capturing all relevant clinical elements (chief complaint, history of present illness, review of systems, physical exam, assessment, and plan) regardless of how long the day has been. This consistency matters for:
Continuity of care when other providers need to review records
Coding accuracy and the revenue it supports
Legal protection in cases where thorough documentation is essential
Quality metrics tied to clinical outcomes and reimbursement programs
Strengthening Doctor-Patient Relationships
Perhaps the most significant, and least quantifiable, benefit of AI medical scribes is what happens to the human dynamics of a clinical encounter when documentation is taken off the physician's plate.
When doctors aren't typing or dictating, they maintain eye contact. They face their patients instead of screens. They pick up on nonverbal cues they might otherwise miss. They ask follow-up questions that a note-focused visit might cut short.
This human dimension of care matters clinically, not just emotionally. Research consistently shows that stronger therapeutic relationships correlate with better medication adherence, more accurate histories, and improved patient outcomes. 57% of healthcare organizations identify reducing administrative burdens through automation as the most significant opportunity for AI adoption and improved patient interaction is a central reason why.
Improving Workflow Efficiency and Hospital Productivity
At a system level, AI scribes compress the time between encounter and documentation. Notes that previously took 30–60 minutes to complete post-visit are generated in real time. This means:
Faster patient turnover without sacrificing documentation quality
Reduced end-of-day note backlog, which is a major source of "pajama time"
More accurate same-day billing submission, reducing revenue cycle delays
Better staffing utilization, as physicians and support staff spend less time on clerical tasks
AI Medical Scribe Requirements: What You Need to Get Started
Technical Requirements
The good news: modern AI scribes are designed for minimal infrastructure. Most require only:
A microphone-enabled device: smartphone, tablet, or laptop
A stable internet connection: for cloud-based processing
EHR credentials and integration setup: typically handled during onboarding
HIPAA-compliant audio processing environment: usually guaranteed by the vendor
Some enterprise deployments may involve more complex on-premises or hybrid cloud configurations, particularly for large health systems with strict IT governance requirements.
Implementation Timeline
One of the most common questions about AI scribes is how long implementation takes. The honest answer depends on scale and integration complexity:
Deployment Size | Typical Timeline |
|---|---|
Individual practitioner | 1–3 days |
Small practice (2–10 providers) | 1–2 weeks |
Mid-size group practice | 2–6 weeks |
Hospital or health system | 4–12 weeks |
Most vendors offer structured onboarding with dedicated support, template configuration, EHR integration testing, and physician training. The faster implementations tend to involve cloud-based tools with out-of-the-box EHR connectors rather than custom on-premises deployments.
Training and Adoption
AI scribes typically involve a brief voice training period in which the system learns to recognize an individual clinician's speech patterns and terminology preferences. This is usually completed within the first few sessions of use, not a weeks-long process.
More important than technical training is change management: helping physicians build new documentation habits and trust the AI's output. Most experienced implementers recommend:
Starting with lower-complexity note types before specialty-specific documentation
Establishing a clear review-and-edit workflow so physicians stay in the loop
Setting expectations that the AI generates a draft that the clinician approves, not a finished product to be signed without review
Collecting ongoing feedback to refine templates and improve accuracy over time
Choosing the Right AI Scribe: Hospitals vs. Private Practices
For Hospitals and Health Systems
Large healthcare organizations have different priorities than individual practitioners. Key considerations include:
Enterprise EHR integration with systems like Epic, Cerner, or Meditech at scale
Multi-specialty template libraries that cover the full breadth of clinical services
Role-based access controls and centralized user management
Analytics dashboards for measuring documentation quality and clinician time savings
Vendor support SLAs appropriate for 24/7 clinical operations
Scalability to onboard hundreds or thousands of providers
Recent major health system deployments include Cleveland Clinic's enterprise rollout of Ambience Healthcare's AI platform and John Muir Health's implementation as the first major system with fully integrated ambient AI in Epic workflows.
For Private Practices and Independent Clinicians
Smaller practices typically prioritize different factors:
Cost-effectiveness: monthly per-provider pricing models are preferable to large upfront capital investments
Ease of setup: solutions that work with existing smartphones and tablets without additional hardware
Minimal IT overhead: cloud-based tools managed by the vendor, not internal IT
Flexible customization: the ability to configure templates without needing technical expertise
Responsive support: smaller practices rarely have dedicated implementation teams and need vendor-provided guidance
Pro Tip: For solo practitioners and small practices evaluating AI scribes, prioritize vendors that offer free trials with real patient encounters, not just demos. How the AI handles your specialty, your documentation style, and your EHR is the only evaluation that matters.
The Cost and ROI of Implementing AI Medical Scribes
Pricing models vary significantly across vendors. Most cloud-based AI scribes are priced on a per-provider, per-month subscription basis, ranging from roughly $100 to $500 per provider depending on features and scale.
The ROI calculation, however, typically makes a compelling case:
Reduced transcription and human scribe costs: Human scribes cost $30,000–$60,000+ per year in salary and benefits. AI scribes eliminate or significantly reduce that expense.
Improved billing capture: More complete documentation leads to fewer missed charges and more accurate coding, studies estimate this can recover 3-5% of annual revenue in practices with previously incomplete documentation.
Physician retention: The cost of replacing a physician who leaves due to burnout is estimated at $500,000–$1 million when accounting for recruitment, onboarding, and lost productivity. Reducing burnout has a direct financial value.
Additional patient capacity: When documentation is faster, physicians can see more patients without extending their hours.
AI Medical Scribe Data Security: What Clinicians Need to Know
Security concerns are among the most frequently cited barriers to AI scribe adoption and they're legitimate concerns worth addressing seriously.
HIPAA Compliance Is the Baseline
Any AI scribe used in a U.S. clinical setting must comply with HIPAA's Privacy and Security Rules. In practice, this means:
Protected health information (PHI) cannot be stored or transmitted without appropriate safeguards
The vendor must execute a Business Associate Agreement (BAA) with the covered entity
Access logs must be maintained and available for audit
Data breach notification procedures must be in place
A vendor that won't sign a BAA or can't provide documentation of HIPAA compliance is not a viable option for clinical use, regardless of other features.
Questions to Ask Every Vendor
Before deploying any AI scribe, get explicit answers to:
Is audio recording stored after note generation and if so, for how long and with what access controls?
Is data used to train the AI model and if so, is PHI anonymized before use?
Where is data stored geographically, and does the infrastructure meet HITRUST or SOC 2 Type II standards?
What is the incident response protocol if a breach occurs?
How are user access and permissions managed across a multi-provider practice?
These aren't adversarial questions, any reputable vendor will have clear, documented answers.
AI Medical Scribe Legal Implications and Certification
Who Is Responsible for the Note?
This is the most important legal question surrounding AI scribe use, and the answer is unambiguous: the clinician who signs the note is always responsible for its accuracy and completeness. AI scribes generate drafts, not final documentation. The physician's review and signature constitutes attestation that the note accurately represents the clinical encounter.
This means:
Physicians should never sign AI-generated notes without reviewing them
Any errors in the final signed note are the clinician's responsibility, not the vendor's
Practices should have clear policies specifying the review standard expected before attestation
Certification and Training Requirements
There is currently no federal certification requirement for AI medical scribe use in the United States. However, several professional organizations have issued guidance:
The American College of Physicians has published frameworks for responsible AI use in clinical documentation
Many state medical boards are actively developing guidance on AI-assisted documentation
Some health systems require internal training and competency verification before allowing providers to use AI scribes independently
This regulatory landscape is evolving rapidly. Clinicians and practice administrators should monitor guidance from their relevant specialty societies and state boards.
Future Trends in AI Medical Scribing
The AI medical scribe market is one of the fastest-growing segments in health technology. The global market reached $1.53 billion in 2025 and is projected to reach $5.08 billion by 2030, a 27.2% compound annual growth rate driven by expanding telehealth, rising regulatory documentation requirements, and continued clinician demand.
Several trends are shaping where the technology goes next:
Ambient AI Becoming Standard of Care
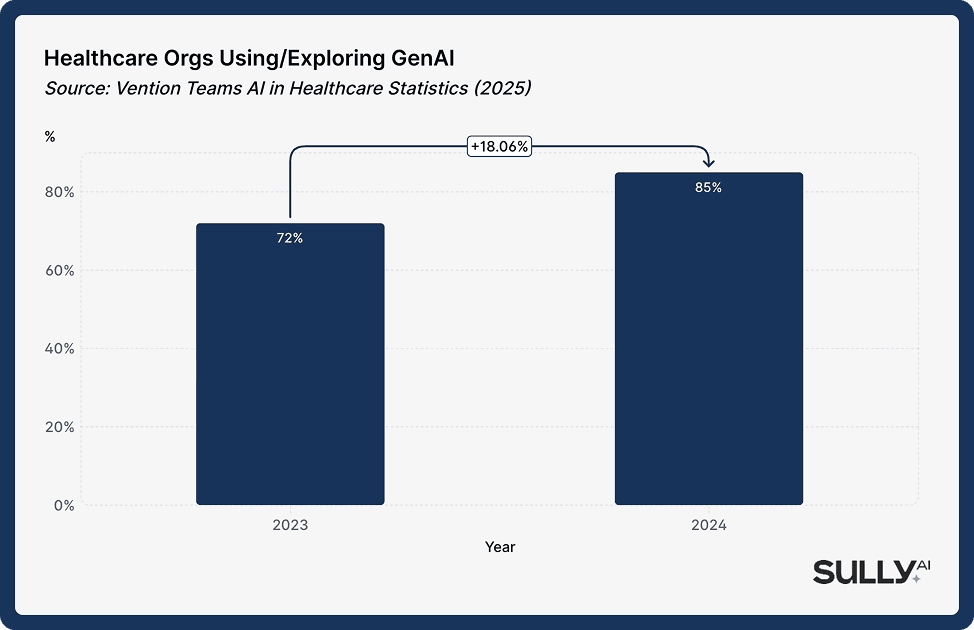
What was an early-adopter technology in 2022–2023 is becoming standard infrastructure today. The share of healthcare organizations that have adopted or explored generative AI rose from 72% in Q1 2024 to 85% by year-end, a pace that suggests ambient AI scribing will be a baseline expectation rather than a differentiator within a few years.
Predictive Documentation and Clinical Decision Support
The next frontier goes beyond documentation. Emerging AI scribe platforms are integrating predictive analytics that suggest potential diagnoses based on symptoms discussed, flag drug interactions mentioned during the encounter, or prompt documentation of elements required for specific quality measures. This shifts AI from a passive recorder to an active clinical intelligence layer.
Multimodal and Multilingual Capabilities
Leading AI scribe vendors are expanding multilingual support to accurately capture and document encounters in multiple languages, a critical capability for health systems serving diverse patient populations. Some platforms are also beginning to incorporate non-verbal cues and contextual signals beyond speech.
The AI Medical Team
Forward-thinking health systems are moving beyond standalone AI scribes toward integrated AI medical teams, interconnected AI agents that handle the full administrative and clinical support workflow. Sully's platform reflects this direction with coordinated AI agents covering reception, scribing, coding, triage, and patient communication within a unified system.
Frequently Asked Questions
What is an AI medical scribe?
An AI medical scribe is a software system that uses artificial intelligence and natural language processing to automatically generate structured clinical notes from physician-patient conversations in real time. Unlike traditional transcription, AI scribes understand clinical context and format documentation into EHR-ready notes without manual input from the clinician.
How does an AI medical scribe work?
AI scribes use ambient listening technology to capture clinical encounters via a microphone-enabled device. The audio is processed by NLP algorithms that identify clinically relevant content, apply appropriate medical structure (SOAP notes, assessment and plan, etc.), and generate a draft note for physician review, typically within seconds of the encounter ending. The clinician reviews, edits if needed, and approves the note for EHR entry.
Is patient data safe with AI medical scribes?
Reputable AI scribe platforms are HIPAA-compliant by design, using end-to-end encryption, multi-factor authentication, and strict access controls. Before deploying any platform, practices should confirm the vendor will sign a Business Associate Agreement (BAA), request documentation of HIPAA and security certifications, and clarify data retention policies, particularly whether audio recordings are stored post-transcription.
What are the AI medical scribe requirements for getting started?
Most AI scribes require only a microphone-enabled smartphone or tablet, a stable internet connection, and EHR credentials for integration setup. Enterprise deployments in large health systems may require more complex IT configuration, but individual practitioners and small practices can typically be operational within days.
Do AI medical scribes replace human scribes?
AI scribes automate the documentation process for the vast majority of routine clinical encounters, significantly reducing or eliminating the need for human scribes in most practice settings. Some organizations retain human oversight for complex cases, legal proceedings, or high-stakes documentation scenarios where human judgment adds critical value.
How much does an AI medical scribe cost?
Most cloud-based AI scribes are priced on a per-provider, per-month subscription basis, typically ranging from $100 to $500 depending on features, specialty customization, and scale. This compares favorably to human scribes, which typically cost $30,000–$60,000+ per year in salary, benefits, and management overhead.
Can AI scribes adapt to different medical specialties?
Yes. Leading AI scribe platforms offer specialty-specific customization covering primary care, internal medicine, emergency medicine, psychiatry, surgery, pediatrics, and many others. Templates can be further customized to individual physician preferences for terminology, note structure, and included documentation elements.
What are the legal implications of using an AI medical scribe?
The clinician who reviews and signs the AI-generated note bears full responsibility for its accuracy and completeness. AI scribes generate drafts, the physician's attestation is what makes the note a legal medical record. Practices should establish clear review policies and stay current with evolving guidance from specialty societies and state medical boards on AI-assisted documentation.
Sources
[1] Grand View Research: U.S. AI in Medical Scribing Market Report 2033. https://www.grandviewresearch.com/industry-analysis/us-ai-medical-scribing-market-report
[2] Towards Healthcare: AI in Medical Scribing Market Size and Growth, 2025–2035. https://www.towardshealthcare.com/insights/ai-in-medical-scribing-market-sizing
[3] The Business Research Company / EIN Presswire: AI Medical Scribe Software Market to Hit $5.08B by 2030. https://www.einpresswire.com/article/893307711/ai-medical-scribe-software-market-to-hit-5-08b-by-2030-tbrc-exclusive-insights
[4] Vention Teams: AI in Healthcare 2025 Statistics: Market Size, Adoption, Impact. https://ventionteams.com/healthtech/ai/statistics
[5] American Medical Association: U.S. Physician Burnout Hits Lowest Rate Since COVID-19 (2024 data). https://www.ama-assn.org/practice-management/physician-health/us-physician-burnout-hits-lowest-rate-covid-19
[6] American Medical Association: Physician Burnout Statistics 2024: Latest Changes and Trends. https://www.ama-assn.org/practice-management/physician-health/physician-burnout-statistics-2024-latest-changes-and-trends
[7] Tebra / The Intake: Primary Care Under Pressure: What 2025 Burnout Data Reveals. https://www.tebra.com/theintake/staffing-solutions/primary-care-physician-burnout-data
[8] Tebra / The Intake: Physician Burnout by Specialty 2025. https://www.tebra.com/theintake/staffing-solutions/independent-practices/physician-burnout-by-specialty
[9] Coherent Solutions: Benefits and Pitfalls of AI Medical Scribe and Transcription. https://www.coherentsolutions.com/insights/benefits-and-pitfalls-of-ai-medical-scribe-and-transcription-solutions
[10] EurekAlert / Mass General Brigham: Ambient documentation technologies reduce physician burnout (JAMA Network Open, Aug 2025). https://www.eurekalert.org/news-releases/1095044
[11] Mediontech: 2025 Healthcare AI Revolution: 68% of physicians report increased AI use for documentation. https://www.mediontech.com/2025-healthcare-ai-revolution-it-doesnt-replace-doctors-it-gives-them-superpowers/amp/
[12] American Medical Association: How Much Is Physician Burnout Costing Your Organization? https://www.ama-assn.org/practice-management/physician-health/how-much-physician-burnout-costing-your-organization
[13] MGMA: Physician Burnout Still a Major Factor Even as Unexpected Turnover Eases (2024). https://www.mgma.com/mgma-stat/physician-burnout-still-major-factor-even-as-unexpected-turnover-eases
[14] DataIntelo: AI Medical Scribe Software Market Research Report 2033. https://dataintelo.com/report/ai-medical-scribe-software-market
TABLE OF CONTENTS
Hire your
Medical AI Team
Take a look at our Medical AI Team
AI Receptionist
Manages patient scheduling, communications, and front-desk operations across all channels.
AI Scribe
Documents clinical encounters and maintains accurate EHR/EMR records in real-time.
AI Medical Coder
Assigns and validates medical codes to ensure accurate billing and regulatory compliance.
AI Nurse
Assesses patient urgency and coordinates appropriate care pathways based on clinical needs.