From reading a chest CT in seconds to flagging early-stage cancer markers that conventional methods would miss, artificial intelligence in diagnostics is compressing timelines, increasing accuracy and giving clinical teams a decisive edge in patient outcomes.
If your organization is still treating AI as a pilot program rather than a core clinical infrastructure investment, this guide will help you understand the use of AI in diagnostics better.
Key Takeaways
The market is surging and the window for early adoption is now: The global AI in diagnostics market reached $1.94 billion in 2025 and is projected to hit $10.28 billion by 2034, a 20.37% CAGR, with North America commanding 58% of current revenue share.
Imaging AI has crossed the mainstream threshold: 90% of healthcare organizations now report at least partial implementation of AI tools for medical imaging, and the FDA has authorized over 692 AI-enabled medical devices, 77% of them in radiology.
AI improves speed and accuracy simultaneously: AI triage systems in radiology can flag X-rays 20–30 minutes faster than standard worklist order, while deep learning frameworks are achieving diagnostic classification accuracies of up to 94.95% across multimodal imaging datasets.
Physician adoption accelerated dramatically in 2024: 66% of physicians used health AI in 2024, an increase of 78% from 2023, signaling that clinical resistance is giving way to operational expectation.
ROI arrives fast: Organizations implementing AI healthcare solutions are seeing an average return of $3.20 for every $1 invested, typically within 14 months, making the business case as strong as the clinical one.
Why AI Diagnostics in Medicine Is a Strategic Imperative
The diagnostic process is the foundation of every care pathway. When that foundation is slow, inaccurate, or resource-constrained, everything downstream suffers, patient outcomes, provider satisfaction, operational margins, and institutional reputation. For large hospitals and health systems serving 500 or more employees and patients, the stakes are exponentially higher.
Research from the National Academy of Medicine estimates that diagnostic errors affect roughly 12 million Americans each year in outpatient settings alone, and contribute to approximately 40,000–80,000 deaths annually. These aren't edge cases, they're systemic failures that AI diagnostics is uniquely positioned to address.
The Hidden Costs of Diagnostic Delay and Error
Every day a diagnosis is delayed or missed is a day the care plan is wrong. For high-volume clinical environments, these delays compound into serious operational and financial consequences:
Increased readmissions: Patients discharged without a confirmed diagnosis are significantly more likely to return within 30 days, triggering penalties under CMS value-based care programs.
Downstream resource waste: Unnecessary follow-up imaging, lab repeats, and specialist referrals drive up per-episode costs in ways that a faster, more accurate initial diagnosis would eliminate.
Clinician burnout: Radiologists, pathologists, and emergency physicians face crushing interpretive workloads. In fact, 92% of healthcare leaders agree that automation is critical for addressing staff shortages, per the 2024 Royal Philips Future Health Index.
Liability exposure: Missed diagnoses and delayed treatment create malpractice risk, particularly in high-acuity specialties like oncology, cardiology, and neurology.
Key Insight: The question is no longer whether AI diagnostics provides value — the clinical and financial evidence is overwhelming. The real question is how quickly your organization can move from selective piloting to enterprise-level integration.
What's Driving AI Diagnostics Advancement in 2026
The current acceleration of AI diagnostics advancement is being driven by four converging forces.
First, deep learning architectures have matured significantly, enabling models trained on millions of annotated images to generalize across patient populations with high reliability.
Second, the regulatory environment has caught up: the FDA has now authorized over 692 AI-enabled devices, predominantly in radiology and cardiology, providing legal clarity for clinical deployment.
Third, EHR interoperability has improved, allowing AI engines to ingest structured and unstructured clinical data at the point of care.
Fourth, ambient documentation tools, such as Sully.ai’s AI medical scribe, are handling the administrative load that previously crowded out clinical decision-making, freeing physicians to act on AI-generated insights rather than fight documentation backlogs.
AI Diagnostics Applications Across Clinical Specialties

Understanding where AI diagnostics delivers the most impact helps clinical leadership prioritize investment and integration sequencing. The current deployment landscape spans virtually every diagnostic specialty, but several domains show especially high maturity and evidence density.
Radiology and Medical Imaging
Radiology is where AI diagnostics has established its deepest clinical roots. A systematic review published in eClinicalMedicine in 2025, covering 140 studies across AI implementation, effectiveness, and cost, found consistent evidence of improvements in diagnostic accuracy and reductions in interpretation time when AI tools are deployed alongside radiologists. Pilot programs at Level I trauma centers report that AI-flagged X-rays are read 20–30 minutes faster on average than standard worklist order, a difference that can determine whether a stroke or hemorrhage patient survives with full function or not.
In lung cancer screening, AI platforms like Median Technologies' eyonis™ LCS, which demonstrated statistically significant improvements in early-stage detection across two major clinical trials, are setting a new standard for sensitivity and specificity in CT analysis. When combined with a human reader, AI triage can double the detection rate of malignant nodules, according to chest/abdominal CT research published in late 2025.
Pathology and Oncology
In pathology, AI is transforming the analysis of tissue samples, whole-slide images, and cellular morphology. Deep learning frameworks integrating pathology and radiology imaging have demonstrated classification accuracies of up to 94.95% with F1 Scores up to 94.85% across multimodal medical imaging datasets, per a 2025 Frontiers in Medicine study. In oncology specifically, AI-powered cancer diagnostic tools have reached a 93% match rate with expert tumor board recommendations, enabling individualized treatment recommendations at scale.
AI is also being deployed in precision genomics, analyzing tumor DNA methylation patterns, identifying molecular subgroups in cancers like medulloblastoma, and predicting chemotherapy response, capabilities that fundamentally shift oncology from population-based to individualized care.
Cardiology and Neurology
In cardiology, machine learning models analyzing ECG data have reached classification accuracy rates exceeding 90% in identifying heart disease, while AI systems have demonstrated the ability to rule out heart attacks at twice the speed of humans with 99.6% accuracy. The real-time analysis of continuous cardiac monitoring data enables a shift from episodic assessment to true continuous vigilance.
Neurology has seen similarly compelling results. A 2025 multicenter prospective study conducted across 67 inpatient medical organizations in Moscow evaluated AI performance in detecting intracranial hemorrhage (ICH) on brain CT across more than 3,400 studies. The study demonstrated that AI-assisted radiologists outperformed both standalone AI and unassisted radiologists, confirming the "augmented clinician" model as the highest-performing configuration for neuroimaging diagnosis. AI stroke diagnosis technology is now being implemented across stroke centers in multiple countries, with the UK committing to nationwide deployment.
Emergency Medicine and Critical Care
Emergency medicine is perhaps where AI diagnostics delivers the most immediate life-or-death value. AI algorithms analyzing vital signs, imaging, and lab results can flag patients at risk of sepsis, acute kidney injury, or stroke before traditional clinical signals become obvious. This predictive capability transforms triage from a reactive process into a proactive one. For large emergency departments managing hundreds of daily encounters, AI-driven clinical decision support systems mean that high-acuity patients get escalated faster; and low-acuity patients aren't unnecessarily consuming intensive resources.
How AI Diagnostics Works: The Technology Behind Faster, More Accurate Results
For clinical and operational leaders evaluating AI diagnostics platforms, understanding the underlying mechanisms builds confidence and informs procurement decisions.
Machine Learning and Deep Learning in Diagnostic Imaging
The core of modern AI diagnostics is deep learning, specifically convolutional neural networks (CNNs) and transformer-based architectures trained on vast annotated medical imaging datasets. These models learn to identify patterns, the precise radiodensity profile of a pulmonary nodule, the cellular morphology of a carcinoma, the signal irregularities in an arrhythmia, with a consistency and granularity that exceeds human visual processing at scale.
What makes current-generation models particularly powerful is their multimodal capability. Modern foundation models can now process both images and text simultaneously, enabling them to cross-reference imaging findings with clinical notes, lab values, and patient history in real time. A 2025 Nature Scientific Reports study demonstrated that integrating radiology and pathology imaging through AI significantly improves diagnostic accuracy, segmentation precision, and reconstruction fidelity compared to single-modality approaches.
Natural Language Processing and Clinical Documentation
Beyond imaging, AI diagnostics increasingly incorporates natural language processing (NLP) to extract diagnostic signals from unstructured clinical documentation, physician notes, discharge summaries, referral letters. NLP engines can identify symptom clusters, flag missing workup steps, and surface relevant historical findings that might otherwise be buried in voluminous records.
This is where AI medical platforms create compounding value: by automating documentation with ambient AI scribes, they simultaneously free physicians to engage more deeply with clinical findings and ensure that the structured data feeding diagnostic AI is complete, accurate, and current.
Pro Tip: The quality of AI diagnostic output is directly dependent on the quality of the data it ingests. Organizations that invest in ambient documentation tools and EHR optimization before deploying imaging AI will see substantially better diagnostic AI performance from day one.
Predictive Analytics and Clinical Decision Support
Predictive analytics represents the forward-looking dimension of AI diagnostics, moving from "what is wrong now" to "what will go wrong next." Johns Hopkins Hospital's collaboration with Microsoft Azure AI, for example, deployed AI algorithms trained on electronic health records, imaging, and genomic data to predict disease progression, readmission risk, and treatment response, enabling genuinely proactive clinical intervention. About 65% of U.S. hospitals now report using predictive analytics or AI-driven predictive models in their operations, with 79% relying on models embedded in their EHR systems.
Enhancing Diagnostic Accuracy: What the Evidence Shows
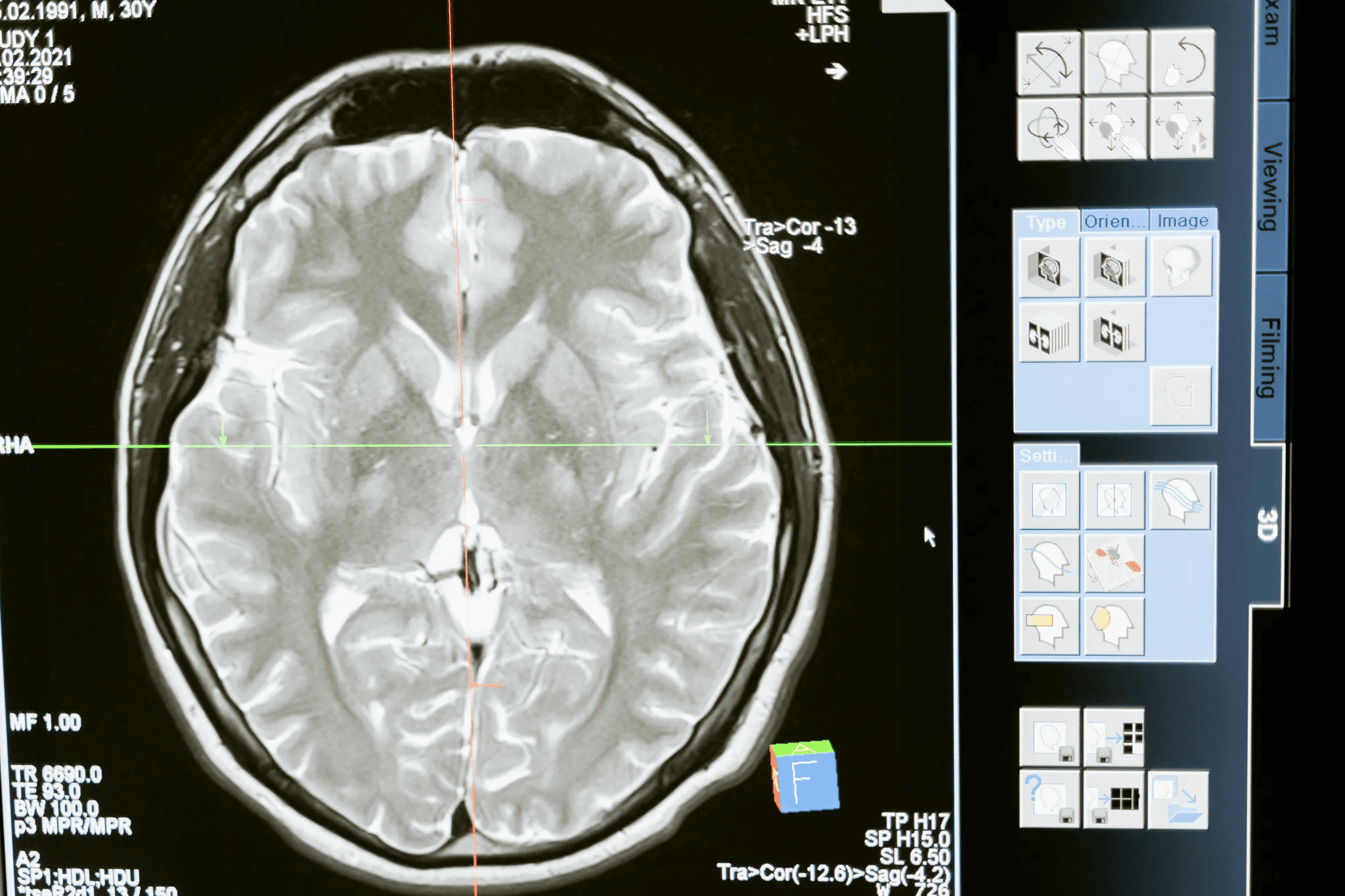
The accuracy case for AI diagnostics is no longer built on promising pilot studies. It is increasingly grounded in prospective, multicenter, real-world clinical evidence across multiple specialties.
AI as Augmentation, Not Replacement
The single most important finding from 2024–2025 clinical research is that the optimal configuration is augmented, AI plus clinician, rather than autonomous AI alone. The eClinicalMedicine systematic review found that AI was viewed most favorably and performed most reliably when deployed as a "second reader", a support tool that surfaces findings for clinician confirmation rather than a replacement for expert judgment. The Moscow ICH study reinforced this conclusion, showing AI-assisted radiologists outperforming both standalone AI and unassisted radiologists on intracranial hemorrhage detection.
Reduction in Diagnostic Errors and Missed Findings
One of AI's most documented clinical contributions is the reduction in missed diagnoses, findings that would be overlooked in standard review due to reader fatigue, cognitive load, or the inherent limitations of unaided visual inspection. In mammography, AI has achieved documented reductions in both false positives and false negatives, with some studies reporting improvements of up to 9% in early breast cancer detection compared to standard radiologist assessment. In dermatology, deep learning models classify skin lesions and identify melanoma with accuracy rivaling experienced dermatologists.
In ophthalmology, AI tools analyzing retinal scans enable early diagnosis of diabetic retinopathy and macular degeneration at scales that make population-wide screening economically viable for the first time.
The Accuracy Ceiling and Its Implications
It's important to contextualize AI accuracy claims honestly. A 2024 meta-analysis of 83 studies found that generative AI models achieved an overall diagnostic accuracy of 52.1%, comparable to non-expert physicians but significantly below expert specialists. This is not a failure of AI; it's a design specification. AI diagnostics performs best when targeted at specific, well-defined tasks within a supervised clinical workflow, not as a generalist autonomous diagnostician.
The appropriate deployment model is one where AI handles the high-volume, pattern-recognition-intensive workload, and human clinicians provide the contextual judgment, ethical oversight, and patient communication that algorithms cannot replicate.
The bottom line: AI doesn't eliminate diagnostic variability — it floors it. By standardizing the baseline performance of your diagnostic workflows, AI ensures that every patient gets the equivalent of a highly trained specialist's pattern recognition, regardless of which clinician is on shift.
The Role of AI Medical Scribes in Diagnostic Workflows
A diagnostic decision is only as good as the data informing it. This is where AI medical scribes, a category that Sully.ai's AI Scribe leads in clinical settings, become a foundational element of any AI diagnostics strategy. Documentation quality directly impacts diagnostic quality, and the two cannot be decoupled.
How AI Scribes Improve Diagnostic Data Quality
AI medical scribes capture the clinical encounter in real time using ambient voice recognition, NLP-powered data extraction, and EHR-native integration. Each step serves a diagnostic function:
Real-time transcription: Every symptom, medication, and clinical observation articulated during the encounter is captured immediately, eliminating the recall bias that degrades retrospective documentation.
Structured data extraction: NLP algorithms parse clinical language into coded diagnostic fields, ensuring that symptoms map to ICD-10 categories, medications are flagged for interactions, and abnormal findings trigger appropriate follow-up workflows.
Contextual cross-referencing: AI scribes compare new encounter data against the patient's existing records, surfacing historical findings that are directly relevant to current diagnostic questions and reducing duplicate testing.
EHR integration: Because documentation is completed during, not after, the encounter, the data feeding downstream AI diagnostic tools is current, complete, and structured correctly from the outset.
The Time Savings That Compound Into Better Diagnostics
Hospitals deploying AI scribe technology consistently report significant reductions in administrative time, with physicians reclaiming two or more hours per clinical day that were previously consumed by documentation. This matters diagnostically because physician burnout is a primary driver of diagnostic error. Fatigued clinicians miss findings. Clinicians who have mental bandwidth, because AI has absorbed their documentation load, engage more deeply with the clinical picture.
Pro Tip: When evaluating AI scribe platforms for your health system, prioritize those that integrate natively with your EHR and structure output as codified diagnostic data, not just free-text transcription. The downstream diagnostic AI depends on it.
AI Diagnostics and Personalized Medicine
The convergence of AI diagnostics with genomics and precision medicine represents one of the most transformative frontiers in modern clinical care.
Genomic Analysis at Scale
AI's capacity to analyze genomic data at scale is enabling a new class of diagnostic insights that were computationally impractical even five years ago. Machine learning models can now sift through millions of genetic variants across large patient populations, identifying combinations of single-nucleotide polymorphisms (SNPs) associated with elevated disease risk before any clinical symptom appears.
In oncology, AI analysis of hundreds of exomes in medulloblastoma cases has identified specific molecular subgroups that allow physicians to calibrate treatment doses with a precision that population-based protocols cannot achieve.
Treatment Matching and Predictive Therapeutics
Beyond diagnosis, AI is reshaping treatment selection by matching patients with therapies optimized for their individual genetic and molecular profiles. In cancer care, AI can analyze the genomic profile of a tumor to identify which targeted therapies or immunotherapies are most likely to achieve response, moving beyond the trial-and-error approach that has historically characterized oncology treatment.
This is where AI diagnostics intersects with AI-powered clinical support tools like Sully.ai's AI Consultant, which provides real-time clinical decision support informed by the full breadth of a patient's diagnostic data. The result is a clinical workflow where diagnosis, treatment matching, and documentation happen in a continuous, AI-augmented loop, rather than three separate, disconnected processes.
AI Diagnostics Comparison: Platform Capabilities for Health Systems
Understanding what to look for when evaluating AI diagnostics platforms ensures that procurement decisions align with clinical outcomes rather than vendor marketing claims.
Capability | What to Look For | Why It Matters |
|---|---|---|
Imaging Analysis | FDA-cleared algorithms; multimodality support (CT, MRI, X-ray, pathology slides) | Regulatory clarity and clinical coverage breadth |
Real-Time Processing | Sub-minute turnaround on flag generation; live triage integration | Time-critical in emergency and acute care settings |
Documentation Integration | Native EHR integration; NLP-structured output; ambient capture | Diagnostic data quality depends on documentation quality |
Compliance & Security | HIPAA-compliant architecture; SOC 2 certification; audit trail | Non-negotiable for enterprise health system deployment |
Explainability | Visual confidence maps; reason codes; override workflows | Required for clinician trust and emerging regulatory requirements |
Outcome Analytics | Population-level diagnostic performance dashboards; A/B benchmarking | Enables continuous quality improvement and ROI measurement |
Ethical, Legal, and Compliance Considerations for Enterprise Deployment
Deploying AI diagnostics in a large health system is not simply a clinical or technology decision, it's a governance decision with significant legal, ethical and regulatory dimensions.
HIPAA, Data Privacy, and Security
Every AI diagnostic system deployed in a U.S. healthcare setting must operate within HIPAA's Privacy and Security Rules, which govern how protected health information (PHI) is used, stored, and transmitted. This is foundational, not optional. Enterprise AI deployments require data processing agreements, Business Associate Agreements (BAAs) with every AI vendor in the data flow, and security architectures that segregate diagnostic AI training data from live patient records.
FDA Regulatory Pathways
AI-enabled medical devices in the U.S. must navigate FDA regulatory pathways appropriate to their risk classification. The FDA's 692-device cleared inventory, 77% in radiology, provides a growing catalog of approved tools, but clinical leaders must verify that the specific algorithms deployed carry appropriate clearance for their intended use and patient population. Deploying cleared devices outside their labeled indication creates both clinical and regulatory risk.
Liability and Clinical Accountability
One of the most consequential unresolved questions in healthcare AI is liability allocation when an AI-assisted diagnosis is wrong. Current legal frameworks generally assign liability to the clinician who acted on the AI output, not to the AI vendor. This makes clinician training, override documentation, and audit trail integrity mission-critical elements of any enterprise AI diagnostics deployment.
The Future of AI Diagnostics: What's Coming Next
The trajectory of AI diagnostics advancement in 2026 and beyond points toward three converging developments that will redefine what diagnostic medicine looks like in the next decade.
Multimodal Foundation Models
The shift from narrow, task-specific AI models to large multimodal foundation models — analogous to large language models in natural language processing, but trained on imaging, genomic, clinical note, and lab data simultaneously — is accelerating. These models can contextualize findings across data types in ways that narrow models cannot, enabling a form of synthetic clinical reasoning that approaches the integrative thinking of an experienced specialist. Early deployments in academic medical centers are already demonstrating performance gains on complex, multi-system presentations where narrow AI has historically struggled.
Continuous Ambient Monitoring
Point-in-time diagnostics will increasingly give way to continuous monitoring architectures — AI engines that analyze streaming data from wearables, implanted sensors, and bedside devices to detect diagnostic signals before they manifest as acute presentations. For large health systems, this shifts the diagnostic burden from episodic high-intensity encounters to ongoing low-intensity signal processing — with AI handling the volume and surfacing only the findings that warrant human attention.
Autonomous Diagnostics for Underserved Populations
Perhaps the most societally significant near-term application is the deployment of AI diagnostic tools in underserved and resource-constrained settings where specialist access is limited. AI-powered mobile health applications and telemedicine services are enabling screening, diagnosis, and care initiation for patients in rural and low-resource communities, effectively democratizing access to the diagnostic expertise that currently concentrates in urban academic medical centers.
The good news is that the infrastructure investment required to build these capabilities is already paying for itself. With an average ROI of $3.20 per dollar invested and typical payback within 14 months, AI diagnostics is not just the clinically superior path, it's the financially responsible one.
Frequently Asked Questions
What is AI diagnostics in medicine?
AI diagnostics refers to the use of artificial intelligence technologies, including machine learning, deep learning, and natural language processing, to analyze clinical data and assist in identifying diseases and conditions. These systems process medical images, lab results, genomic data, and clinical notes to surface diagnostic signals faster and with greater consistency than unaided human review. AI diagnostics does not replace physician judgment; it augments it by handling high-volume pattern recognition tasks and surfacing findings for clinician confirmation.
How accurate is AI in medical diagnostics?
Accuracy varies significantly by task and deployment context. AI diagnostic systems have demonstrated 90-95% accuracy for specific, well-defined tasks such as detecting intracranial hemorrhage on brain CT, classifying skin lesions, or identifying diabetic retinopathy from retinal scans.
In broader applications, a 2024 meta-analysis found generative AI diagnostic accuracy at 52.1%, comparable to non-expert physicians. The most reliable configuration is AI-assisted clinicians, where the combined accuracy of human expertise plus AI pattern recognition consistently outperforms either alone.
What are the most common AI diagnostics applications in hospitals?
The highest-deployment applications as of 2026 are: radiology and medical imaging AI (90% of healthcare organizations have at least partial implementation), ambient clinical documentation (100% of large health systems report some usage per the AMA's 2024 report), predictive analytics for patient risk stratification (65% of U.S. hospitals), and pathology AI for tissue analysis. Cardiology, neurology, dermatology, and oncology are the clinical specialties with the deepest AI diagnostics penetration.
How does AI diagnostics integrate with existing hospital systems?
Modern AI diagnostics platforms are designed for EHR-native integration via FHIR APIs and HL7 standards, allowing them to ingest data from and return structured output to existing clinical systems without requiring workflow disruption. The most effective implementations connect imaging AI directly to PACS (Picture Archiving and Communication Systems), ambient documentation tools directly to EHR workflows, and predictive analytics engines to care management platforms.å
What are the regulatory requirements for AI diagnostics in the U.S.?
AI-enabled diagnostic tools in the U.S. are regulated as medical devices under FDA jurisdiction. The regulatory pathway, typically 510(k) clearance or De Novo authorization for lower-risk AI tools, depends on the device's intended use and risk classification.
As of late 2023, the FDA has authorized 692 AI-enabled medical devices, primarily in radiology. Additionally, all deployments must comply with HIPAA privacy and security requirements, and organizations must execute Business Associate Agreements with AI vendors that process PHI.
How can a large health system get started with AI diagnostics?
The most effective starting point is a diagnostic data readiness assessment, evaluating EHR data completeness, imaging archive quality, documentation practices, and existing clinical workflows. From there, prioritize two or three high-value use cases where AI has the strongest clinical evidence base and where your organization has the data infrastructure to support it (radiology AI and ambient documentation are typically the best initial targets). Engage clinical champions in each affected specialty early, establish clear performance benchmarks, and plan for a 6–12 month integration and change management runway before expecting full operational impact.
Sources
[1] Precedence Research: Artificial Intelligence in Diagnostics Market Size 2025 to 2034. https://www.precedenceresearch.com/artificial-intelligence-diagnostics-market
[2] TempDev: 65 Key AI in Healthcare Statistics (2025). https://www.tempdev.com/blog/2025/05/28/65-key-ai-in-healthcare-statistics/
[3] IntuitionLabs: AI in Radiology: 2025 Trends, FDA Approvals & Adoption. https://intuitionlabs.ai/articles/ai-radiology-trends-2025
[4] DemandSage: AI in Healthcare Statistics 2025: Adoption & Market Size. https://www.demandsage.com/ai-in-healthcare-stats/
[5] Fortune Business Insights: AI in Healthcare Market Size, Share & Growth Report 2026–2034. https://www.fortunebusinessinsights.com/industry-reports/artificial-intelligence-in-healthcare-market-100534
[6] Dialog Health: AI in Healthcare Statistics: Comprehensive List for 2025. https://www.dialoghealth.com/post/ai-healthcare-statistics
[7] Docus AI: AI in Healthcare Statistics 2025: Overview of Trends. https://docus.ai/blog/ai-healthcare-statistics
[8] The Lancet / eClinicalMedicine: Artificial intelligence for diagnostics in radiology practice: a rapid systematic scoping review (2025). https://www.thelancet.com/journals/eclinm/article/PIIS2589-5370(25)00160-9/fulltext
[9] Frontiers in Medicine: Deep learning-based image classification for AI-assisted integration of pathology and radiology in medical imaging (2025). https://www.frontiersin.org/journals/medicine/articles/10.3389/fmed.2025.1574514/full
[10] Nature Scientific Reports: Deep learning-based image classification for integrating pathology and radiology in AI-assisted medical imaging (2025). https://www.nature.com/articles/s41598-025-07883-w
[11] PubMed Central: Standalone AI Versus AI-Assisted Radiologists in Emergency ICH Detection: A Prospective, Multicenter Diagnostic Accuracy Study (2025). https://pmc.ncbi.nlm.nih.gov/articles/PMC12386909/
[12] Scispot: AI Diagnostics: Revolutionizing Medical Diagnosis in 2026. https://www.scispot.com/blog/ai-diagnostics-revolutionizing-medical-diagnosis-in-2025
[13] BreastCancer.org: Artificial Intelligence and Breast Cancer Screening. https://www.breastcancer.org/screening-testing/artificial-intelligence
[14] NCBI Bookshelf: 2025 Watch List: Artificial Intelligence in Health Care. https://www.ncbi.nlm.nih.gov/books/NBK613808/
[15] MDPI / Clinics and Practice: Artificial Intelligence in Clinical Medicine: Challenges Across Diagnostic Imaging, Clinical Decision Support, Surgery, Pathology, and Drug Discovery (2025). https://www.mdpi.com/2039-7283/15/9/169
[16] National Academy of Medicine: Improving Diagnosis in Healthcare. https://www.ncbi.nlm.nih.gov/books/NBK338596/
[17] CMS: Value-Based Programs Overview. https://www.cms.gov/medicare/value-based-programs/value-based-programs
[18] FDA: Artificial Intelligence and Machine Learning (AI/ML)-Enabled Medical Devices. https://www.fda.gov/medical-devices/software-medical-device-samd/artificial-intelligence-and-machine-learning-aiml-enabled-medical-devices
[19] HHS: HIPAA for Professionals. https://www.hhs.gov/hipaa/index.html
[20] Sully.ai: AI Medical Assistant Platform. https://www.sully.ai/
[21] Sully.ai: AI Scribe Technology: How It's Revolutionizing Medical Documentation. https://www.sully.ai/blog/ai-scribe-technology-how-it-s-revolutionizing-medical-documentation
[22] Biomedcentral / Surgical and Experimental Pathology: Unveiling the future: the impact of artificial intelligence in diagnostic pathology (2025). https://surgexppathol.biomedcentral.com/articles/10.1186/s42047-025-00197-1
[23] **PMC / Health Science Reports:**The Impact of Artificial Intelligence on Healthcare: A Comprehensive Review (2025). https://pmc.ncbi.nlm.nih.gov/articles/PMC11702416/
[24] AI Multiple: Top 6 Radiology AI Use Cases for Improved Diagnostics. https://research.aimultiple.com/radiology-ai/
[25] PMC: Physician Burnout and Diagnostic Error. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7749428/
TABLE OF CONTENTS
Hire your
Medical AI Team
Take a look at our Medical AI Team
AI Receptionist
Manages patient scheduling, communications, and front-desk operations across all channels.
AI Scribe
Documents clinical encounters and maintains accurate EHR/EMR records in real-time.
AI Medical Coder
Assigns and validates medical codes to ensure accurate billing and regulatory compliance.
AI Nurse
Assesses patient urgency and coordinates appropriate care pathways based on clinical needs.